Introduction:
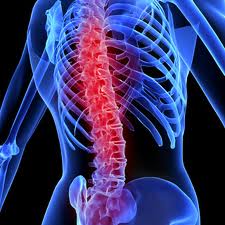
Spinal cord injuries usually begin with a blow that fractures or dislocates your vertebrae, the bone disks that make up your spine. Most injuries don’t sever your spinal cord. Instead, they cause damage when pieces of vertebrae tear into cord tissue or press down on the nerve parts that carry signals. In a complete spinal cord injury, the cord can’t relay messages below the level of the injury. As a result, you are paralyzed below the level of injury. In an incomplete injury, you have some movement and sensation below the injury. A spinal cord injury is a medical emergency. Immediate treatment can reduce long-term effects. Later treatment usually includes medicine and rehabilitation therapy.
Improved emergency care for people with spinal cord injuries and aggressive treatment and rehabilitation can minimize damage to the nervous system and even restore limited abilities. Respiratory complications are often an indication of the severity of spinal cord injury. About one-third of those with injury to the neck area will need help with breathing and require respiratory support. The steroid drug methyl prednisolone appears to reduce the damage to nerve cells if it is given within the first 8 hours after injury. Rehabilitation programs combine physical therapies with skill-building activities and counseling to provide social and emotional support.
Spinal cord injuries are classified as either complete or incomplete. An incomplete injury means that the ability of the spinal cord to convey messages to or from the brain is not completely lost. People with incomplete injuries retain some motor or sensory function below the injury. A complete injury is indicated by a total lack of sensory and motor function below the level of injury. People who survive a spinal cord injury will most likely have medical complications such as chronic pain and bladder and bowel dysfunction, along with an increased susceptibility to respiratory and heart problems. Successful recovery depends upon how well these chronic conditions are handled day to day.
The prevalence of spinal cord injury is not well known in many large countries. In some countries, such as Sweden and Iceland, registries are available. According to new data collected by the Christopher and Dana Reeve Foundation, in the US, there are currently 1.3 million individuals living with spinal cord injuries- a number five times that previously estimated in 2007. 61% of spinal cord injuries occur in males, and 39% in females. The average age for spinal cord injuries is 48 years old. There are many causes leading to spinal cord injuries. These include motor vehicle accidents (24%), work-related accidents (28%), and sporting / recreation accidents (16%), and falls (9%). [1]
More than 80 percent of the world’s population lives in the more than 100 developing countries (Soubbotina 2000), but we know little about SCI form this part of the world. There can be many reasons such as constraints of resources and research funding, priority of curable diseases over incurable SCI lesions, and lack of general interest in the medical community to address a prolonged and often permanent disability.
Justification of the Study
SCI results in complications affecting nearly all systems of the body, leading to an increased morbidity and mortality in this group of patients.
The complications profile reported from the developing countries are similar to that of the developed world with notably increased incidence (Chacko et al. 1986). The high frequency of preventable complications indicates a general lack of awareness in the health care professionals as well as inability of the patients to adhere to a life long prevention regime. In developing countries the problem of pressure ulcers is more critical because of lack of access to specialized technologies and adequate medical and pressure ulcer risk assessment. In some cases these pressure ulcers even prove fatal for the patient (Rathore et al. 2008, Gosselin and Coppotelli 2005). Urinary tract infections also occur with a very high frequency with possible etiological factors as indicated by Rathore and colleagues, 2007. Another important factor may be inability to use disposable catheters for clean intermittent catherization due to the expenses involved. The reported incidence of thromboembolic disorders like pulmonary embolism and deep vein thrombosis in the SCI population in West is high (Weingarden 1992, Green 2003) despite adequate use of thromboprophylaxis. A vast majority of SCI patients in the developing world are not given standard thromboprophylaxis. The reason for this disparity is not clear although many mechanisms have been proposed. These include genetic factors, low prevalence of obesity and heart failure in the developing world, and possibly early mobilization and massage of lower limbs and role of dietary factors (Kalstky et al. 2000, Bagaria et al. 2006, Aito et al. 2007, Rathore et al. 2008).
In Bangladesh there are many disabilities caused by spinal injuries. In addition, accident is a major cause of death in Bangladesh. The complication of SCI is started from sport of injury due to the miss handling of patient, improper moving and handling. Even in hospital improper moving and handling by untrained staff. There are very scarcities of facilities to manage accidental cases especially spinal injury. Only tertiary levels of hospitals provide medical support for the SCI patients. Perhaps it is important to know the situation of the specialized hospital for their readiness to provide quality care for SCI patients. The study will provide information for improving the medical services of the hospitals to provide care to spinal injury patients in Bangladesh.
Given the above factors, there are a number of arenas that need to be addressed in order to adequately influence the service provider and to promote a stronger operational commitment from all levels of societies so that they might recognize and meet the specific needs and priorities for proper knowledge about spinal injury patient management and right to have proper knowledge ensuring these as their health rights.
Literature Review
Spinal cord injury (SCI) is a devastating neurological injury, resulting in varying degrees of paralysis, sensory loss and sphincter disturbance which are permanent and irreversible in cases. It was labeled as “an ailment not to be treated” in the Edwin Smith papyrus 5000 years ago (Feldman and Goodrich 1999). Unfortunately not much has changed, in many parts of the world known as the underdeveloped countries. SCI has been studied in detail in the Developed world, and thousands of manuscripts have been published in the last few decades. These include large scale epidemiologic surveys, multicenter research on interventions in acute SCI, reports on complications from acute and chronic SCI, results of rehabilitation interventions and functional outcomes. But all this covers only a part of the world population.
SCI results in complications affecting nearly all systems of the body, leading to an increased morbidity and mortality in this group of patients. The complications profile reported from the developing countries are similar to that of the developed world with notably increased incidence (Chacko et al. 1986). The high frequency of preventable complications indicates a general lack of awareness in the health care professionals as well as inability of the patients to adhere to a life long prevention regime. In developing countries the problem of pressure ulcers is more critical because of lack of access to specialized technologies and adequate medical and pressure ulcer risk assessment.
In some cases these pressure ulcers even prove fatal for the patient (Rathore et al. 2008, Gosselin and Coppotelli 2005). Urinary tract infections also occur with a very high frequency with possible etiological factors as indicated by Rathore and colleagues, 2007. Another important factor may be inability to use disposable catheters for clean intermittent catherization due to the expenses involved. The reported incidence of thromboembolic disorders like pulmonary embolism and deep vein thrombosis in the SCI population in West is high (Weingarden 1992, Green 2003) despite adequate use of thromboprophylaxis. A vast majority of SCI patients in the developing world are not given standard thromboprophylaxis. Still the frequency of PE and DVT in these patients, especially from Asian region is low in many studies (Toe 1978, Lee et al. 2000, Rathore et al. 2008). The reason for this disparity is not clear although many mechanisms have been proposed. These include genetic factors, low prevalence of obesity and heart failure in the developing world, and possibly early mobilization and massage of lower limbs and role of dietary factors (Kalstky et al. 2000, Bagaria et al. 2006, Aito et al. 2007, Rathore et al. 2008). Other reported complications include spasticity, depression, contractures, gastrointestinal complications, heterotrophic ossification and pain.
There are no established national trauma or SCI registries in the developing countries. Similarly there is no population based data on SCI available from majority of the developing world countries. This is complicated by the fact that medical record keeping is poorly managed in most of the hospitals (Thanni and Kehinde 2006). Most of the data are single center hospital based surveys representing less than 15 countries of the developing world (Toe 1978, Chacko et al. 1986, Maharaj 1996, Otom et al. 1997, Levy et al. 1998, Igun et al. 1999, Deconinck 2003, Quinones et al. 2002, Singh et al. 2003, Gosselin and Coppotelli 2005, Shrestha et al. 2007, Rathore et al. 2008, Rahimi-Movaghar et al. 2009). Many of them are retrospective surveys. The general demographics of SCI in the developing world share some similarities with the epidemiological pattern reported from the developed countries. For example SCI is primarily a disease of the young males. But there are many important differences as well that need to be considered. (Divanoglou and Levi 2009). The reverse is true for most of the developing countries (Chacko et al. 1986, Maharaj 1996, Singh et al. 2003, Rathore et al. 2008).
Because of the prevalent social customs in the underdeveloped regions, majority of the patients with SCI are distressed at the time of their injury (Rathore et al.2008). This goes to the advantage of the patient as after discharge from the hospital, (Kreuter 2000), but this isn’t the case for most of the developing countries.
Most of the patients in the developed world have incomplete cervical spine injury at presentation. In contrast the commonest pattern reported from the developing world is of complete paraplegia (Chacko et al. 1986, Maharaj 1996, Singh et al. 2003, Rathore et al. 2008). Possible causes of this disparity are discussed in the next section. Immobilization and log roll of a suspected SCI patient at the trauma site is of utmost importance as it prevents further neurological deterioration and cord compression (Shooman and Rushambuza 2009).
Pre Hospital trauma care, first aid at site and infrastructure for transport of spinal trauma patients are inadequate in most of the developing countries (Solagberu et al. 2009, Nguyen et al. 2008). Ambulance rescues services, if any, are available in major cities only. Most of the patients are initially managed by the by standers, with no training in first aid. (Singh et al. 2003, Shrestha et al. 2007, Rathore et al. 2008).
People with SCI are at risk of chest complications because of a number of factors which include: paralysis of ventilatory muscles affecting breathing and coughing capability relative broncho-constriction; excess secretions due to relative parasympathetic system dominance (from reduced sympathetic function in tetraplegics); ventilation/perfusion mismatch from reduced mobility that may exacerbate hypoxia during inter-current illness.
In individuals with tetraplegia, symptomatic bradycardia and, of more concern, asystolic cardiac arrest, are well recognized during the acute phase. This is due to the loss of sympathetic activity with preservation of parasympathetic (vagal) activity. Significant bradycardia usually resolves several weeks after injury, but this mechanism can complicate anesthetic and chest care in chronic tetraplegia, particularly in hypoxia or during suctioning. In individuals with high spinal cord lesions (above mid-thoracic level (T7)), hypotension (eg 0/50) and low or relatively low pulse rate (eg 40–50 bpm) can be physiologically ‘normal’ for that level of spinal cord lesion and are still compatible with effective tissue perfusion. Hypotension from other causes needs to be distinguished carefully from this picture. Overzealous fluid resuscitation or transfusion can cause pulmonary oedema and increased morbidity/mortality. It is helpful to ascertain individuals’ normal resting vital signs before planning intervention. Individuals with SCI at or above T6 level are at risk of autonomic dysreflexia (AD) – an excessive autonomic response to stimuli below the level of the SCI, such as a blocked catheter or faecal impaction. This is an acute and life-threatening condition which all physicians should be aware of.
Sensory loss will complicate the presentation of acute illness in individuals with SCI as the history will not necessarily include localizing symptoms or pain, and localizing signs may not be present.
The great majority of individuals with SCI also have impairments in bladder function but this will depend on the grade and level of injury. Urinary tract infections are one of the most common complications following spinal cord injury and may require hospitalisation. The goals of bladder management are to preserve the upper tracts, minimize lower tract complications and be compatible with the individual’s lifestyle. In the main, patients are followed up at their spinal cord injury centre and have ongoing assessment of urological needs. Many patients are maintained on intermittent self-catheterisation (ISC) regimens, which may be impossible to maintain during acute illness. In this case, it may be appropriate to pass an indwelling catheter if the admission is short. However, long-term indwelling urethral catheters can lead to complications such as infection or urethral stricture. In the longer term, it is preferable to reestablish them, if possible, on their normal bladder routine, in liaison with their regular team. A common scenario is the patient with incomplete SCI who has some spontaneous voiding but retains a residual volume which gradually increases: this can eventually lead to complications if not appropriately managed.
Spinal cord injury has a profound impact on the function of the large bowel and on maintenance of faecal continence. Stool transit through the bowel is slowed, placing individuals at high risk of constipation, especially where morphine or codeinerelated drugs or anticholinergics are used to control pain or other symptoms in intercurrent illness. Sensory and motor control of the anorectum is impaired and therefore individuals will be unable to feel the need to evacuate the bowel, or control the process of defaecation. Without intervention, individuals will be incontinent of faeces and chronically constipated, with all the secondary complications these imply, including the potential risk of autonomic dysreflexia, in patients with lesions above the level of T5–6.
There are no established national trauma or SCI registries in the developing countries. Similarly there is no population based data on SCI available from majority of the developing world countries. This is complicated by the fact that medical record keeping is poorly managed in most of the hospitals (Thanni and Kehinde 2006). Most of the data are single center hospital based surveys representing less than 15 countries of the developing world (Toe 1978, Chacko et al. 1986, Maharaj 1996, Otom et al. 1997, Levy et al. 1998, Igun et al. 1999, Deconinck 2003, Quinones et al. 2002, Singh et al. 2003, Gosselin and Coppotelli 2005, Shrestha et al. 2007, Rathore et al. 2008, Rahimi-Movaghar et al. 2009). Many of them are retrospective surveys. The general demographics of SCI in the developing world share some similarities with the epidemiological pattern reported from the developed countries. For example SCI is primarily a disease of the young males. But there are many important differences as well that need to be considered. Motor vehicle accidents are the leading causes of death in the developed countries followed by falls (Divanoglou and Levi 2009). The reverse is true for most of the developing countries (Chacko et al. 1986, Maharaj 1996, Singh et al. 2003, Rathore et al. 2008). Diving and sports injuries are another important cause of traumatic SCI in the Western world (Boden and Jarvis 2009) but this has rarely been reported from the developing countries. Among the non traumatic SCI, spinal tuberculosis is still an important cause in the underdeveloped countries of the world (Turgut 2001), while it is rarely seen in the developed countries nowadays.
Because of the prevalent social customs in the underdeveloped regions, majority of the patients with SCI are married at the time of their injury (Rathore et al.2008). This goes to the advantage of the patient as after discharge from the hospital, the spouse remains the only and most dedicated care giver in many cases. The divorce rates after SCI are high in the developed world (Kreuter 2000), but this isn’t the case for most of the developing countries.
Most of the patients in the developed world have incomplete cervical spine injury at presentation. In contrast the commonest pattern reported from the developing world is of complete paraplegia (Chacko et al. 1986, Maharaj 1996, Singh et al. 2003, Rathore et al. 2008). Possible causes of this disparity are discussed in the next section.
Plain radiographs can miss fractures, especially facet fractures. The detailed evaluation of a suspected SCI needs advanced radiological imaging techniques like Computerized Tomographic (CT)-scan and Magnetic Resonance Imaging (MRI), to see the extent of damage to the vertebral column, spinal cord and asses the spinal stability (Winter and Pattani 2008).
Radiology is not well established and advanced imaging techniques are not available in many of the hospitals in the developing world (Udosen et al. 2007, Hitimana et al. 2009 ,Standertskjöld 2009). It has been estimated that more than half of the low income countries do not have established neuro rehabilitation and neuroradiology services (Salinas and Medina 2006). Management based on plain X-rays of the spine often results in treatment failure and prolonged periods of immobilization and morbidity for the patient.
Spinal units were established in the West as early as World War II; these units were dedicated to the treatment and rehabilitation of SCI patients in order to manage their needs in a comprehensive manner (Guttmann 1979). In many developed countries regional and national model SCI centers are working for the last 50 years. There are only few centers established in the developing world catering for a small population. The ones which are available many a times don’t have all the members of a standard multidisciplinary rehabilitation team available (Rathore et al. 2008).
As a result most of the SCI in the developing world are managed in the neurosurgical, orthopedic and even in general surgical wards (Nwankwo and Katchy 2003, Udosen et al. 2007) with no established protocols for SCI management and rehabilitation. In many cases the treating physician/surgeon lacks the skills of spinal instrumentation/fixation and conservative management. Moreover a case of orthopedic or general surgery takes precedence over a SCI as “there is not much to offer to a SCI patient”.
SCI management doesn’t end with spinal instrumentation or a decision to pursue a conservative management regime. SCI rehabilitation is the only intervention that ensures a successful community reintegration of a SCI patient as an active member. In the developed world it is a continuum of care available to most, if not all SCI patients. Spinal Cord Injury Medicine is established as a subspecialty in many parts of the developed world.
Rehabilitation medicine is poorly developed in most of the developing countries and “confused with physiotherapy, rather than with a concept of multidisciplinary approach” (Rathore et al. 2007). The number of specialists trained in rehabilitation medicine or in spinal cord injury management is very small in many developing countries and in many places they don’t exist (Haig et al. 2009). In many places orthopedic surgeons and physical therapists are running the department of rehabilitation medicine. This approach addresses only a few aspects like exercises, mobility and gait training and use of gait aids. Other equally and sometimes more important aspects like bladder and bowel training, psychological assessment, skin care, sexual dysfunction and fertility management, addressing vocational concerns, peer counseling and recreational therapy are either neglected or tactfully avoided. In many cases false reassurances are given regarding outcome and prognosis (Rathore et al. 2008).
This is a reason that many patients in the developing world do not have access to adequate and appropriate rehabilitation services necessary for community re-integration even though initial surgical management is adequate.
Research question
What is the current status of health services for spinal injury patients in Dhaka Medical College hospitals in Dhaka city of Bangladesh?
General Objective
To assess the status of health services for spinal injury patients in the Dhaka Medical College Hospital of Dhaka city of Bangladesh.
Specific Objectives
- To find out the service providers in the hospital for providing services for spinal injury patients
- To explore the training status of the service providers
- To know the situation of the equipment of the hospital to provide service
- To examine the situation of the logistics and medicine available to provide service
- To know the situation of operation theatre and ward for spinal injury patients
Operational Definition:
Knowledge: Information, understanding and skill that a person has acquired through education or experience about the fact.
Perception: Awareness, a way and the ability to see, hear or understanding something
Attitude: Behaving towards, a way of thinking about somebody or something
Study Design & Methods
A cross sectional hospital based descriptive study was conducted in Dhaka Medical College Hospital hospitals in Dhaka city. The objective of such study design aimed to focus cross cutting issues that come across for assessing the knowledge about the status of health services for spinal injury patients.
Sampling Techniques
In compliance with the study objectives, selected 100 service providers were selected purposively from Dhaka Medical College Hospital hospitals in Dhaka city.
Sampling formula
The sample size was calculated on basis of the following formula:
Z2 x pq
d 2
Where,
n = Sample size estimate
Z = Z for level of significance alpha (at 0.05 level of significance value of Z is 1.96)
p= 50%
q= 1-p
d= acceptable margin of error (.05)
Actual sample size was
(n) = Z² pq/d²
= (1.96) ² × 0.5 × 0.5/ (0.05) ²
= 3.84 × 0.25 / 0.0025
=385
Using this formula, the sample respondents are approximately 384. But due to limitation of time and budgetary constraint number of respondents was limited within 100 respondents from two hospitals in Dhaka city. The study utilized random sampling method to identify the respondents from the hospital.
Study population
Total number of respondents participated in the study was 100 in number. It was also found that all of the respondents were from different Professional, social strata and from different backgrounds. The respondents of the study were service providers; basically nurses, doctors from both indoor and outdoor.
Location of the Study:
The study was conducted in Dhaka city and more specifically in the Dhaka city Metropolitan area. The study sites was Shahid Suhrawardi. hospitals of Dhaka city and the population of the study will be the 100 service providers including 80 nurses and 20 doctors from both indoor and outdoor.
Inclusion criteria
- Service provider from Shahid Suhrawardi Hospital in Dhaka city.
- Willing to participate in the study and to provide information about existing facilities and knowledge required for the study.
Exclusion criteria
- Unwilling to participate in the study
- Not fallen under the random sampling procedure and not presented in the interview.
Data Collection, Management & Analysis
As the research was based on primary data, and explorative in nature, data was collected through a structured questionnaire. Data was collected through a structured questionnaire and checklist prepared by the interviewer and approved by the examination board. Baseline information on socio-demographics, knowledge, attitude and practice towards SCI patient will be collected from the study participants through interviewer-administered questionnaire through face to face interview. Questions will be asked about the status of health services for the spinal injury patient. Explore the training status of the service providers, know the situation of the equipment of the hospital to provide service, examine the situation of the logistics and medicine available to provide service and know the situation of operation theatre and ward for spinal injury patients
Data analysis was carried out using SPSS (version 14). Categorical variables were reported as proportion, while continuous variables were reported as means and standard deviations when distributions are considered approximately normal. Whereas, the impact of socio demographic factors of the adolescent and how to improve the situation was assessed through the survey. The analyzed data was also presented in tables, graphs, charts and bars to meet the specific objective and enhance the understandings.
Data Collection Procedure
After explaining the purpose of the study to the respondents, data was collected through face to face interview using English/Bengali structure questionnaire.
Conduction of the study, quality control and monitoring
The data was collected from selected areas by the interviewer. The collected data was checked and verified by the investigator at the end of the work every day. Any inaccuracy and inconsistency was corrected in the next working day. However, cross checking of the collected data was done randomly.
Data Processing and data analysis
The data entry process started immediately after the completion of data collection. The collected data was checked, verified and then entered into the computer. Only fully completed datasheet was entered into the computer for the final analysis. The analysis was carried out with the help of SPSS (Statistical Package for Social Science) Windows software program.
Ethical consideration
Prior to the commencement of this study, the research protocol was approved by the research committee (Local Ethical committee). The aims and objectives of the study along with its procedure, risks and benefits of this study was explained to the respondents in easily understandable and then informed consent was taken from each respondents. Then it was assured that all information and records will be kept confidential and the procedure will be used only for research purpose and the findings will be helpful for developing policy to increase the spinal injury related knowledge among the service providers.
Informed Consent
A well and clearly understood inform consent form will be filled in up by the respondents and interviewer. However, translations might be carried out after the according to the need of the respondents. This ensures that each of participants will get the information they need to make an informed decision.
Variables
The study comprised of both independent and dependent variable
Dependant Variable:
Current status of health services of the patients with spinal injury.
Independent Variables:
- Age
- Education
- Duration of job
- Training received
- Number of service providers in the hospital for providing services for spinal injury patients
- Training status of the service providers
- Situation of the equipment of the hospital to provide service
- Situation of the logistics and medicine available to provide service
- Situation of operation theatre and ward for spinal
Results
Demographic status of the respondents:
Respondent Status: Before starting the result analysis, the gender status and age of the respondents were calculated. It was evident from the study that, the study was conducted in Dhaka Medical College hospital in Dhaka to assess the current health services of the patients with spinal injury. Total number of respondents participated in the study was 100 in number. It was also found that all of the respondents were from different social strata and from different backgrounds. The respondents of the study were service providers; basically nurses, doctors and from both indoor and outdoor.
Table 1: Age of the respondents
Age of the respondent
| Frequency | Percent | |
| 21-30 years | 9 | 9.0 | |
| 31-40 years | 68 | 68.0 | |
| 41-50 years | 17 | 17.0 | |
| 51-60 years | 6 | 6.0 | |
| Total | 100 | 100.0 | |
While addressing the age of the respondents from the study, it was observed from the study that, the age range of the respondents was limited within 21 to 60 years. While it was found that 68% of the respondents’ age was in between 31-40 years, and 9% of the respondents were aged in between 21-30 years. 17% respondent’s age was in between the age limit of 41-50 years. It was also found that only 6% respondent’s were from the age group of 51-60 years.
Table 2: Sex of the Respondent
| Sex of the Respondent | Frequency | Percent |
Male | 33 | 33.0 |
Female | 67 | 67.0 |
Total | 100 | 100.0 |
In order to know about the gender status among the respondents, it was found from the study that 33% of the respondents were male and 67% respondents were found female. This number implies, women are much familiar with the care of spinal cord injury patients in the study area.
Table 3: Occupational status of the respondents
| Occupation | Frequency | Percent |
| Doctor | 14 | 14.0 |
| Nurse | 86 | 86.0 |
| Total | 100 | 100.0 |
To know about occupational status of the respondents, about 86% respondents mentioned their occupation as the Nursing. Only 14% respondents among the study population were found as doctors.
Table 4: How long do you working here?
| How long do you working here? | Frequency | Percent |
| 1-5 years | 28 | 28.0 |
| 6-10 years | 23 | 23.0 |
| 11-15 years | 32 | 32.0 |
| 16-20 years | 3 | 3.0 |
| 21-25 years | 14 | 14.0 |
| Total | 100 | 100.0 |
To know about the working experiences among the respondents, it was found that about 28% respondents were found who have been working for 1-5 years. Besides, 23% of the respondents were found who were experienced more than 5 years but below 10 years. 32% of the respondents reported that they have an experience of above 10 years but less than 15 years. Only 3% of the respondents were found whose experience was in between 16-20 years. Another 14% respondents mentioned about their experience which was 21-25 years.
Table 5: What is your position here?
| What is your position here? | Frequency | Percent |
| Senior stuff nurse | 80 | 80.0 |
| Stuff nurse | 2 | 2.0 |
| Medical officer | 6 | 6.0 |
| Interne Doctor | 10 | 10.0 |
| Consultant | 2 | 2.0 |
| Total | 100 | 100.0 |
In order to know the respondents position in the hospital facility, respondents were asked to tell about their position. In response to the query, it was found that most of the respondents (80%) were the Senior Staff nurses, whereas 2% respondents were Staff nurses. 6% of the respondents were found as the medical officers and 10% respondents were found as interne doctors at the hospital facility. Only 2% respondents were found to be as the consultants who were senior most in terms of position of the medical facility.
Table 6: Who is your supervisor here?
| Who is your supervisor here? | Frequency | Percent |
| Nursing super | 80 | 80.0 |
| Medical officer | 1 | 1.0 |
| Dpt.head | 18 | 18.0 |
| Consultant | 1 | 1.0 |
| Total | 100 | 100.0 |
In order to identify the accountability cycle of the study areas (hospitals), and learn about the supervisory role of the staffs as well, it was found that Nursing super is the supervisors of 80% of the respondents. That means, senior staff nurses are accountable to the Nursing super as the person is their supervisor. Only 1 respondent mentioned to be accountable to the medical officer. Other 18% respondents mentioned that departmental head is their supervisor. Only 1 respondent mentioned the consultant as to be the supervisor.
In order know about the respondent’s level of education, it was found that 69% respondents mentioned their educational qualification as up to S.S.C and they also mentioned after this they had the diploma in nursing. Besides, it was also found that 11% of the respondents were educated up to HSC level. Only 3% respondents mentioned there educational qualification up to BA. It was noteworthy that 16% of the respondents were found who possessed an MBBS degree. Only 1% respondent among the whole frequency was found who have a post graduation degree.
Table 7: Did you study further after your basic degree?
| Did you study further after your basic degree? | Frequency | Percent |
| yes | 98 | 98.0 |
| No | 2 | 2.0 |
| Total | 100 | 100.0 |
It was inevitable from the respondent’s opinion that, without medical degree or training, it is not possible to deliver the service to the patients. In aligned with the qualification or basic degree, respondents were asked that whether they have studied after their basic degree or not. It was found that only 98% respondents have studied or studying after receiving their basic degree. However, only 2% respondents mentioned that they did not study after their basic degree.
Table 8: Have your received any training on how to manage spinal injury patients during your job?
| Have received any training on how to manage spinal injury | Frequency | Percent |
| yes | 5 | 5.0 |
| No | 95 | 95.0 |
| Total | 100 | 100.0 |
Respondents were asked to tell about whether they have received any training on how to manage spinal injury patients or not. Responding the query, it was found that, 95% of the respondent did not received any training on how to manage spinal injury patients, whereas only 5% respondents have prior knowledge about the spinal injury patients as they have received training on it.
Table 9: Does your supervisor co-operate you to take care of the patients
| Does your supervisor co-operate you to take care of the patients with spinal injury? | Frequency | Percent |
| yes | 86 | 89.6 |
| No | 6 | 6.3 |
| Often | 4 | 4.2 |
| Total | 96 | 100.0 |
In order to assess the level of cooperation from the supervisor’s end in assisting the respondent to provide care of the patients with spinal injury, it was found that 89.6% of the respondents were found who used to receive co-operation from their supervisors while managing the patients. Only 6.3% respondents mentioned that they did not receive any cooperation from their supervisor while taking care of the patients. Besides, 4.2% respondents mentioned that, their supervisor used to help them often, when it is possible for them to provide spare times for their subordinates. Interestingly, 4% respondents did not reply to the question.
Table 10: Do you have enough trained manpower to support the spinal injury patients
| Do you have enough trained manpower to support the spinal injury patients? | Frequency | Percent |
| yes | 7 | 7.1 |
| No | 91 | 92.9 |
| Total | 98 | 100.0 |
Respondents were also asked to tell whether they think that they have enough trained manpower to manage or support the spinal injury patients or not, and in response to the question it was found that only 7.1% respondents feel that, the existing number of staff or manpower or their skill or training is enough to provide support for the spinal injury patients. Besides, it was found from the study that 92.9% respondents treated their manpower or the skill as insufficient to manage and to provide support for the spinal injury patients.
Table 11: Does the institution have enough equipment for managing its indoor patients?
| Does the institution have enough equipment for managing its indoor patients? | Frequency | Percent |
| yes | 11 | 11.2 |
| No | 87 | 88.8 |
| Total | 98 | 100.0 |
To assess, respondent’s opinion about the existing facilities or equipments for managing the indoor patients, it was found that, only 11.2% of the respondents feels that the existing equipments or facilities are available for providing support and managing the indoor patients. On the other hand it was found that 88.8% respondents think it to be insufficient for managing the patients.
Table 12: What type of equipments do you have in the hospital for supporting the spinal injury patients?
What type of equipments do you have in the hospital for supporting the spinal injury patients? (multiple answers acceptable)
Frequency | Percent | |
| Spinal board for receiving patient | 2 | .3 |
| Resuscitation equipment | 39 | 5.8 |
| Oxygen cylinder | 100 | 14.9 |
| Sucker machine | 98 | 14.6 |
| Ambo bag | 70 | 10.4 |
| Sphygmomanometer | 100 | 14.9 |
| Stethoscope | 100 | 14.9 |
| Thermometer | 100 | 14.9 |
| Portable X-Ray facilities | 59 | 8.8 |
| Others | 2 | .3 |
| Total | 670 | 100.0 |
In order to know about the general equipments which do the respondents have in their hospital for providing support to the spinal injury patients, it was found that, only 2 respondents opinion supported that they have Spinal board for receiving patient in their hospital facility. 39 respondents mentioned Resuscitation equipment as available equipment. All of the respondents mentioned the availability of Oxygen cylinder, Sphygmomanometer, Stethoscope, Thermometer as to be the available equipments for supporting the spinal injury patients. However, 98 respondents mentioned about the availability of Sucker machine and 70 told about the availability of Ambo bag in the hospital facility. 59 respondents also mentioned the availability of Portable X-ray as supporting equipment to the spinal injury patients.
Table 13: What type of facilities do you have in the hospital?
| What type of facilities do you have in the hospital for supporting the spinal injury patients? | Frequency | Percent |
| Emergency Pathological Lab | 88 | 8.6 |
| Orthopedic bed | 59 | 5.8 |
| Physiotherapy department | 90 | 8.8 |
| ECG | 95 | 9.3 |
| Special dressing room | 78 | 7.6 |
| Mini operation theatre | 84 | 8.2 |
| Surgical instruments | 98 | 9.6 |
| Plaster table | 88 | 8.6 |
| Ambulance service | 92 | 9.0 |
| First aid facilities | 94 | 9.2 |
| CT scan | 75 | 7.3 |
| MRI facilities X-ray | 85 | 8.3 |
| Total | 1026 | 100.0 |
In order to know about the facilities, the respondents have in the hospital for supporting the spinal injury patients, it was found that 88 respondents mentioned about the Emergency Pathological Lab, and 59 respondents mentioned about orthopedic bed. 90 respondents told that they have Physiotherapy department in their hospital facility.95 respondents mentioned about having ECG machine and 78 respondents mentioned about having Special dressing room. Mini operation theatre was an available facility to 84 respondents. Surgical instruments and Plaster table was available according to 98 and 88 respondents accordingly. While, 92 respondents mentioned about the availability of Ambulance service it was found that 75 respondents mentioned CT scan as their available facility. 85 respondents illustrated those MRI X-ray facilities as their available service to provide support for the spinal injury patients.
In order to know about the special facilities available in the medical facility, it was found that, 43.7% of the respondents mentioned about having a special operation theater. 3.4% respondents also mentioned that ICU is also available for the spinal injury patients at their hospitals. Almost 50.6% respondents noted that Physical medicine department is available in their hospital. Only 2.3% mentioned that Rehabilitation center is also available in their hospital for supporting spinal injury patients.
Table 14: Does the hospital management take regular Programs on Spinal Injury?
Does the hospital management take regular discussion/seminar/refresher training on spinal injury?
Frequency | Percent | |
| yes | 14 | 14.0 |
| No | 86 | 86.0 |
| Total | 100 | 100.0 |
With a view to assess the role of hospital management to initiate regular discussion/seminar/refresher training on spinal injury, respondents were asked to tell about their experience. In light of the question, it was found that, only 14% respondents mentioned that hospital authority shoulders the responsibility to initiate the regular discussion/seminar/refresher training on spinal injury for promotion of knowledge among the service providers to the spinal injury patients. Hereby, it was also found that 86% respondents did not found any special arrangement by the hospital management to initiate the knowledge promotion and development.
Table 15: Do you think there should be regular training or class should be conducted to increase knowledge on spinal injury?
Frequency | Percent | |
| yes | 88 | 88.0 |
| No | 12 | 12.0 |
| Total | 100 | 100.0 |
Respondents were also asked to provide their opinion on necessity of knowledge building activity, like regular training or class on spinal injury, and in response to this query, it was found that almost 88% respondents mentioned that it is really necessary to initiate knowledge building activities like training and class to increase the knowledge on spinal injury. While 12% respondents mentioned that it is not necessary to conduct regular training or classes to increase the knowledge on spinal injury.
Discussion
There are no established national trauma or SCI registries in the developing countries. Similarly there is no population based data on SCI available from majority of the developing world countries. This is complicated by the fact that medical record keeping is poorly managed in most of the hospitals (Thanni and Kehinde 2006). SCI is primarily a disease of the young males. But there are many important differences as well that need to be considered. (Divanoglou and Levi 2009). Before starting the result analysis, the gender status and age of the respondents were calculated. It was evident from the study that, the study was conducted in two selected hospitals in Dhaka to assess the current health services of the patients with spinal injury. Total number of respondents participated in the study was 100 in number. It was also found that all of the respondents were from different social strata and from different backgrounds. The respondents of the study were service providers; basically nurses, doctors from both indoor and outdoor.
While addressing the age of the respondents from the study, it was observed from the study that, the age range of the respondents was limited within 21 to 60 years. While it was found that 68% of the respondents’ age was in between 31-40 years, and 9% of the respondents were aged in between 21-30 years. 17% respondent’s age was in between the age limit of 41-50 years. It was also found that only 6% respondent’s were from the age group of 51-60 years.
In order to know about the gender status among the respondents, it was found from the study that 33% of the respondents were male and 67% respondents were found female. This number implies, women are much familiar with the care of spinal cord injury patients in the study area. To know about occupational status of the respondents, about 86% respondents mentioned their occupation as the Nursing. Only 14% respondents among the study population were found as doctors.
While discussing about working experiences among the respondents, it was found that about 28% respondents were found who have been working for 1-5 years. Besides, 23% of the respondents were found who were experienced more than 5 years but below 10 years. 32% of the respondents reported that they have an experience of above 10 years but less than 15 years. Only 3% of the respondents were found whose experience was in between 16-20 years. Another 14% respondents mentioned about their experience which was 21-25 years.
In order to know the respondents position in the hospital facility, respondents were asked to tell about their position. In response to the query, it was found that most of the respondents (80%) were the Senior Staff nurses, whereas 2% respondents were Staff nurses. 6% of the respondents were found as the medical officers and 10% respondents were found as interne doctors at the hospital facility. Only 2% respondents were found to be as the consultants who were senior most in terms of position of the medical facility.
In order to identify the accountability cycle of the study areas (hospitals), and learn about the supervisory role of the staffs as well, it was found that Nursing super is there the supervisor of 80% of the respondents. That means, nurses are accountable to the Nursing Super as the person is their supervisor. Only 1 respondent mentioned to be accountable to the medical officer. Other 18% respondents mentioned that the departmental head are their supervisor. Only 1 respondent mentioned the consultant as to be the supervisor.
In order to know about the respondent’s level of education, it was found that 69% respondents mentioned their educational qualification as up to S.S.C and they also mentioned after this they had the diploma in nursing. Besides, it was also found that 11% of the respondents were educated up to HSC level. Only 3% respondents mentioned there educational qualification up to BA. It was noteworthy that 16% of the respondents were found who possessed an MBBS degree. Only 1% respondent among the whole frequency was found who have a post graduation degree.
It was inevitable from the respondent’s opinion that, without medical degree or training, it is not possible to deliver the service to the patients. In aligned with the qualification or basic degree, respondents were asked that whether they have studied after their basic degree or not. It was found that only 98% respondents have studied or studying after receiving their basic degree. However, only 2% respondents mentioned that they did not study after their basic degree.
Pre Hospital trauma care, first aid at site and knowledge about spinal trauma patients are inadequate in most of the developing countries (Solagberu et al. 2009, Nguyen et al. 2008). This is a reason that many patients in the developing world do not have access to adequate and appropriate rehabilitation services necessary for community re-integration even though initial surgical management is adequate. The number of specialists trained in rehabilitation medicine or in spinal cord injury management is very small in many developing countries and in many places they don’t exist (Haig et al. 2009). Respondents were asked to tell about whether they have received any training on how to manage spinal injury patients or not. Responding the query, it was found that, 95% of the respondent did not received any training on how to manage spinal injury patients, whereas only 5% respondents have prior knowledge about the spinal injury patients as they have received training on it.
In order to assess the level of cooperation from the supervisor’s end in assisting the respondent to provide care of the patients with spinal injury, it was found that 86% of the respondents were found who used to receive co-operation from their supervisors while managing the patients. Only 6% respondents mentioned that they did not receive any cooperation from their supervisor while taking care of the patients. Besides, 4% respondents mentioned that, their supervisor used to help them often, when it is possible for them to provide spare times for their subordinates. Interestingly, 4% respondents did not reply to the question.
Respondents were also asked to tell whether they think that they have enough trained manpower to manage or support the spinal injury patients or not, and in response to the question it was found that only 7% respondents feel that, the existing number of staff or manpower or their skill or training is enough to provide support for the spinal injury patients. Besides, it was found from the study that 91% respondents treated their manpower or the skill as insufficient to manage and to provide support for the spinal injury patients.
To assess, respondent’s opinion about the existing facilities or equipments for managing the indoor patients, it was found that, only 11.2% of the respondents feels that the existing equipments or facilities are available for providing support and managing the indoor patients. On the other hand it was found that 88.8% respondents think it to be insufficient for managing the patients.
Hospitals that generally provide service towards the spinal injury patients should have special equipments. Plain radiographs can miss fractures, especially facet fractures. The detailed evaluation of a suspected SCI needs advanced radiological imaging techniques like Computerized Tomographic (CT)-scan and Magnetic Resonance Imaging (MRI), to see the extent of damage to the vertebral column, spinal cord and asses the spinal stability (Winter and Pattani 2008). In order to know about the general equipments which do the respondents have in their hospital for providing support to the spinal injury patients, it was found that, only 2 respondents opinion supported that they have Spinal board for receiving patient in their hospital facility. 39 respondents mentioned Resuscitation equipment as available equipment. All of the respondents mentioned the availability of Oxygen cylinder, Sphygmomanometer, Stethoscope, Thermometer as to be the available equipments for supporting the spinal injury patients. However, 98 respondents mentioned about the availability of Sucker machine and 70 told about the availability of Ambo bag in the hospital facility. 59 respondents also mentioned the availability of Portable X-ray as supporting equipment to the spinal injury patients.
It has been estimated that more than half of the low income countries do not have established neuro rehabilitation and neuro-radiology services (Salinas and Medina 2006). Management based on plain X-rays of the spine often results in treatment failure and prolonged periods of immobilization and morbidity for the patient. Thus, inadequate access to advanced radiological imaging techniques is a common phenomenon in providing support for the patients. In order to know about the facilities, the respondents have in the hospital for supporting the spinal injury patients, it was found that 88 respondents mentioned about the Emergency Pathological Lab, and 59 respondents mentioned about orthopedic bed. 90 respondents told that they have Physiotherapy department in their hospital facility.95 respondents mentioned about having ECG machine and 78 respondents mentioned about having Special dressing room. Mini operation theatre was an available facility to 84 respondents. Surgical instruments and Plaster table was available according to 98 and 88 respondents accordingly. While, 92 respondents mentioned about the availability of Ambulance service it was found that 75 respondents mentioned CT scan as their available facility. 85 respondents illustrated those MRI facilities as their available service to provide support for the spinal injury patients.
In many developed countries regional and national model SCI centers are working for the last 50 years. There are only few centers established in the developing world catering for a small population. The ones which are available many a times don’t have all the members of a standard multidisciplinary rehabilitation team available (Rathore et al. 2008). Moreover a case of orthopedic or general surgery takes precedence over a SCI as “there is not much to offer to a SCI patient”. Thus, the facilities at the workplace are really low there. In order to know about the special facilities available in the medical facility, it was found that, 43.7% of the respondents mentioned about having a special operation theater. 3.4% respondents also mentioned that ICU is also available for the spinal injury patients at their hospitals. Almost 50.6% respondents noted that Physical medicine department is available in their hospital. Only 2.3% mentioned that Rehabilitation center is also available in their hospital for supporting spinal injury patients.
Most of the SCI in the developing world are managed in the neurosurgical, orthopedic and even in general surgical wards (Nwankwo and Katchy 2003, Udosen et al. 2007) with no established protocols for SCI management and rehabilitation. In many cases the treating physician/surgeon lacks the skills of spinal instrumentation/fixation and conservative management. With a view to assess the role of hospital management to initiate regular discussion/seminar/refresher training on spinal injury, respondents were asked to tell about their experience. In light of the question, it was found that, only 14% respondents mentioned that hospital authority shoulders the responsibility to initiate the regular discussion/seminar/refresher training on spinal injury for promotion of knowledge among the service providers to the spinal injury patients. Hereby, it was also found that 86% respondents did not found any special arrangement by the hospital management to initiate the knowledge promotion and development.
The number of specialists trained in rehabilitation medicine or in spinal cord injury management is very small in many developing countries and in many places they don’t exist (Haig et al. 2009). Respondents were also asked to provide their opinion on necessity of knowledge building activity, like regular training or class on spinal injury, and in response to this query, it was found that almost 88% respondents mentioned that it is really necessary to initiate knowledge building activities like training and class to increase the knowledge on spinal injury. While 12% respondents mentioned that it is not necessary to conduct regular training or classes to increase the knowledge on spinal injury.
Conclusion:
In many parts of the developing world, even today SCI is neglected and poorly managed. Research is sparse and data is missing. The demographics, epidemiological pattern of SCI in the developing world is different from the developed world and this should be considered while formulating polices for the SCI in future. Large scale multi center trials or population based surveys are needed to assess the true magnitude of the problem in the developing world. Trauma evacuation protocols need to be developed and pre hospital care of suspected SCI patient should be improved. Regional and national spinal injury centers providing comprehensive treatment and multidisciplinary rehabilitation should be established. There is a need to establish peer support groups to further the cause of SCI in the developing world. Thus there is no alternate of treatment, rehabilitation and support services focusing on physical, emotional, social, psychological and economic aspects to the SCI patients. The health service providers for the SCI patients can therefore play a vital role and can even attempt to reintegrate the SCI patients into social mainstream with their specialized knowledge and care.
Recommendation:
- Generally SCI patients are rarely served in specialized hospitals which are focused on Spinal cord injury care or sometimes, patients are not directly taken there also. As, SCI is emerging and it needs due attention, special care service for SCI is to be initiated, the sooner it’s possible.
- As, “there is not much to offer to a SCI patient” and the facilities at the workplace are really low in the traditional hospitals, so specialized instruments, equipments for proper medical checkup needs to be ensured which will not be focused only upon the orthopedic care or surgery.
- It is necessary to provide the effective current knowledge based training on SCI or specialization based intervention programs and sharing lessons to the service providers and engaging healthcare practitioners in restructuring the healthcare services and for ensuring better care for the SCI patients.
- As, In many cases the treating physician/surgeon lacks the skills of spinal instrumentation/fixation and conservative management, Pre Hospital trauma care, first aid at site, specialized equipments and infrastructure support for spinal trauma patients is to be ensured by establishing protocols for SCI management and rehabilitation.
References:
Aito S, Abbate R, Marcucci R, Cominelli E. 2007. Endogenous risk factors for deep-vein thrombosis in patients with acute spinal cord injuries. Spinal Cord 45(9):627-631.
Bagaria V, Modi N, Panghate A, Vaidya S. 2006. Incidence and risk factors for development of venous thromboembolism in Indian patients undergoing major orthopedic surgery: results of a prospective study. Postgraduate Medical Journal 82(964):136–139.
Boden BP, Jarvis CG. 2009. Spinal injuries in sports. Physical medicine and rehabilitation clinics of North America 20(1):55-68.
Chacko V, Joseph B, Mohanty SP, Jacob T. 1986. Management of spinal cord injury in a general hospital in rural India. Paraplegia 24(5):330-335.
Deconinck H. 2003. The health condition of spinal cord injuries in two Afghan towns. Spinal Cord 41(5):303-309.
Divanoglou A, Levi R. 2009. Incidence of traumatic spinal cord injury in Thessaloniki, Greece and Stockholm, Sweden: a prospective population-based study. Spinal Cord 47(11):796-801.
Feldman RP, Goodrich JT. 1999. The Edwin Smith Surgical Papyrus. Child’s Nervous System 15(6-7):281–284.
Fraser HS, McGrath SJ. 2000. Information technology and telemedicine in sub-saharan Africa. British Medical Journal 321(7259):465-6.
Gosselin RA, Coppotelli C. 2005. A follow-up study of patients with spinal cord injury in Sierra Leone. International Orthopaedics 29(5):330-332.
Green D. 2003. Diagnosis, prevalence, and management of thromboembolism in patients with spinal cord injury. Journal of Spinal Cord Medicine 26(4):329–334.
Guttmann L. 1979. New hope for spinal cord sufferers. Paraplegia 17(1):6-15.
Haig AJ, Im J, Adewole A, Nelson VS, Krabek B. 2009.The practice of physical medicine and rehabilitation in sub-Saharan Africa and Antarctica: a white paper or a black mark? Disability and Rehabilitation 31(13):1031-1037.
Hart C, Williams E. 1994. Epidemiology of spinal cord injuries: a reflection of changes in South African Society. Paraplegia 32(11):709-714.
Hitimana J, Perez M, Kinasha A, Kakande I. 2009.Clinical Presentation and Outcome of, Rwanda. East and Central African Journal of Surgery 14(1):50-56.
Hoque MF, Grangeon C, Reed K. 1999.Spinal cord lesions in Bangladesh: An epidemiological study 1994 – 1995. Spinal Cord 37(12):858-861
Igun GO, Obekpa OP, Ugwu BT, Nwadiaro HC. 1999. Spinal injuries in the Plateau State, Nigeria. East African Medical Journal 76(2):75-79.
Kalstky AL, Armstrong MA, Poggi J. 2000. Risk of pulmonary embolism and/or deep vein thrombosis in Asian Americans. American Journal of Cardiology 85(11): 1334–1337.
Lee HM, Suk KS, Moon SH, Kim DJ, Wang JM, Kim NH. 2000. Deep vein thrombosis after major spinal surgery: Incidence in an East Asian population. Spine 15;25(14):1827-1830.
Levy LF, Makarawo S, Madzivire D, Bhebhe E, Verbeek N, Parry O. 1998.Problems, struggles and some success with spinal cord injury in Zimbabwe. Spinal Cord 36(3):213-218.
Lidal IB, Huynh TK, Biering-Sørensen F. 2007.Return to work following spinal cord injury: A review. Disability and Rehabilitation 15;29(17):1341-1375.
Maharaj JC. 1996. Epidemiology of spinal cord injury in Fiji: 1985- 1994. Spinal Cord 34(9):549-559.
Nguyen TL, Nguyen TH, Morita S, Sakamoto J. 2008. Injury and pre-hospital trauma care in Hanoi, Vietnam. Injury 39(9):1026-1033.
Nwankwo OE, Katchy AU. 2003. Outcome of a 12-week programme for management of the spinal cord injured with participation of patient’s
relations at Hilltop Orthopaedic Hospital, Enugu, Nigeria. Spinal Cord 41(2):129-133.
Nwomeh BC, Lowell W, Kable R, Haley K , Ameh EA. 2006. History and development of trauma registry: lessons from developed to developing countries. World Journal of Emergency Surgery [cited 2009 Dec 2];1:32. Available from http://www.wjes.org/content/1/1/32
Olasode BJ, Komolafe IE, Komolafe M, Olasode OA. 2006. Traumatic spinal cord injuries in Ile-Ife, Nigeria, and its environs. Tropical Doctor 36(3):181-182.
Oluwadiya KS, Olakulehin AO, Olatoke SA, Kolawole IK, Solagberu BA, Olasinde AA, et al. 2005. Pre-hospital care of the injured in South Western Nigeria: A hospital based study of four tertiary level hospitals in three states. Annual Proceedings – Association for the Advancement of Automotive Medicine 49:93-100.
Otom AS, Doughan AM, Kawar JS, Hattar EZ. 1997. Traumatic spinal cord injury in Jordan- An epidemiological study. Spinal Cord 35(4):253-255.
Quinones POM, Nassal M, AlBader KI, Al Muraikhi AE, Al Kahlout SR. 2002. Traumatic spinal cord injury in Qatar: an epidemiological study. Middle East Journal of Emergency Medicine [cited 2009 Dec 2] 2:3. Available from: http://www.hmc.org.qa/mejem/mar2002/origsty/os3.htm
Rahimi-Movaghar V, Saadat S, Rasouli MR, Ganji S, Ghahramani M, Zarei M, et al. 2009. Prevalence of spinal cord injury in Tehran, Iran. Journal of Spinal Cord Medicine 32(4):428-431.
Raja IA, Vohra AH, Ahmed M. 2001. Neurotrauma in Pakistan. World Journal of Surgery 25(9):1230-1237.
Rathore FA, Farooq F, Muzammil S, New PW, Ahmad N, Haig AJ. 2008. Spinal cord injury management and rehabilitation: highlights and shortcomings from the 2005 earthquake in Pakistan. Archives of Physical Medicine and Rehabilitation 89(3):579-585.
Rathore MF, Farooq F, Butt AW, Gill ZA. 2008. An update on spinal cord injuries in October 2005 earthquake in Pakistan. Spinal Cord 46(6):461-462.
Shooman D, Rushambuza R. 2009. Importance of the log roll. Emergency Medical Journal 26(7):539-540.
Singh R, Sharma SC, Mittal R, Sharma A. 2003. Traumatic spinal cord injuries in Haryana: An epidemiological study. Indian Journal of Community Medicine 28(4):184–186.
Tauqir SF, Mirza S, Gul S, Ghaffar H, Zafar A. 2007. Complications in patients with spinal cord injuries sustained in an earthquake in Northern Pakistan. Journal of Spinal Cord Medicine 30(4):373-377.
Thanni LO, Kehinde OA. 2006. Trauma at a Nigerian teaching hospital: pattern and docu-mentation of presentation. African Health Sciences 6(2):104-107.
Toe T. 1978. Spinal injuries in Rangoon, Burma. Paraplegia 16(1):118-120.
Turgut M. 2001. Spinal tuberculosis (Pott’s disease): Its clinical presentation, surgical management, and outcome. A survey study on 694 patients. Neurosurgical Revue 24(1):8-13.
Udosen AM, Ikpeme AI, Ngim NE. 2007. A prospective study of spinal cord injury in the University Of Calabar Teaching Hospital, Calabar, Nigeria: A preliminary report. The Internet Journal of Orthopedic Surgery. [Cited 2009 Dec 2]; 5:1.
Weingarden SI .1992. Deep venous thrombosis in spinal cord injury; overview of the problem. Chest 102(6 Suppl):636S–639S.