Principle observation of this thesis is to discuss and find out Socio Cultural Problems faced by People Living with HIV/AIDS (PLWHAs) in Bangladesh. Social factors like discrimination, stigmatization and rejection have pushed people living with HIV to become desperate and feel helpless, to the extent of giving up their life. They face discrimination and lack of support not only from the society but also from his/ her own family. This thesis explore the socio-cultural problems faced by PLWHAs and change the attitude and thoughts of the people towards PLWHAs.
Introduction
With less than 0.1 percent of the population estimated to be HIV-positive, Bangladesh is a low HIV-prevalence country. The country faces a concentrated epidemic, and its very low HIV-prevalence rate is partly due to prevention efforts, focusing on men who have sex with men (MSM), female sex workers (FSWs), and injecting drug users (IDUs). In Bangladesh the first case of HIV was detected in 1989. According to NASP 2008, Government of Bangladesh source, till December 2008, there were 1495 reported cases of HIV and 476 cases of AIDS, among them 165 died. Last surveillance conducted in 2007 found national prevalence of HIV < 1%, this makes Bangladesh a low prevalence country. However, there are specific socio-cultural conditions that have the potential to increase the vulnerability of the country to HIV/AIDS.
HIV/AIDS prevention programs have successfully reached 71.6 percent of commercial sex workers (CSWs) in Bangladesh, according to the 2005 United Nations General Assembly Special Session (UNGASS) Country Report. However, only 39.8 percent of CSWs reported using a condom with their most recent client, and just 23.3 percent both correctly identified ways of preventing the sexual transmission of HIV and rejected major misconceptions about HIV transmission. Other factors contributing to Bangladesh’s HIV/AIDS vulnerability include cross-border interaction with high-prevalence regions in Burma and northeast India, low condom use among the general population, and a general lack of knowledge about HIV/AIDS and other sexually transmitted infections (STIs). Bangladesh also has a high tuberculosis (TB) burden, with 102 new cases per 100,000 people in 2005, according to the World Health Organization. HIV infects about 0.1 percent of adult TB patients in Bangladesh and HIV-TB co-infections complicate treatment and care for both diseases
Surveillances showed that in central Dhaka HIV prevalence among Injecting Drug Users (IDUs) rose from 1.4% to 7% (up to 10.8% in a particular locality) during last four years. Simultaneously recent Behavioural Surveillance Survey (BSS) data indicate an increase in risk behaviours such as sharing of injecting equipment and a decline in consistent condom use in sexual encounters between IDUs and female sex workers. BSS data also indicate that the IDU population is well integrated into the surrounding urban community, socially and sexually, thus raising concern about the spread of HIV infection. Over the five surveillance rounds conducted in Bangladesh between 1998 and 2004, the total HIV prevalence remained below 1%. According to the data published by National AIDS/STD programme (NASP) on December 1st 2009, the current situation of HIV/AIDS in Bangladesh is shown in the table below:
| As of 2008 | 2009 | As of 2009 | |
| New HIV | 250 | ||
| Total HIV | 1495 | 1745 | |
| New AIDS | 143 | ||
| Total AIDS | 476 | 619 | |
| New AIDS Death | 39 | ||
| Total AIDS Death | 165 | 204 |
Table: Bangladesh HIV data 2009
The epidemics in many countries of South Asia are now entering a new phase. One of the first populations to be affected by HIV in South Asia were injecting drug users. In areas where drug injection has been long established, such as Manipur in north-eastern India, HIV prevalence rates of over 40 percent have been recorded for several years. Several hundred thousand people infected during the explosive start of epidemics are becoming ill and are undergoing treatment. The treatment of infections becomes a great burden for the country concerned, because HIV/AIDS requires long-term and effective medical care, periodical hospital-based care and trained manpower to provide comprehensive healthcare services. For countries where resources are scarce, easy access to treatment and care remain very questionable and prohibitive for many PLWHAs.
In Bangladesh the situation of human rights in relation to PLWHA seems critical. As PLWHAs are not visible, the reality of the human right situation is difficult to estimate. To Human Rights Watch, “People living with HIV/AIDS and those thought to be infected have been imprisoned, assaulted and even murdered. The stigma of AIDS has taken many lives before the disease itself killed them. But the reasons behind the suicides and extent of this have rarely come to our knowledge. Society’s limited understanding of this disease is causing innocent people to pay a terrible price. Increasingly across the world, there are voices questioning in one angle. They question the narrow approach to a single disease, especially the huge financing for AIDS over all else in basic health care. Our approach to this disease needs to change for the sake of our people, our brothers and our sisters who are fighting against odds.
Social factors like discrimination, stigmatization and rejection have pushed people living with HIV to become desperate and feel hopeless, to the extent of giving up their life. They face discrimination and lack of support not only from the society but also from his/ her own family. They are also being confined from friends, scared for losing their jobs. This made them to live in phobia and their condition become worse as they need proper and adequate treatment that could provide them with better life. Most of these people are not getting proper medical and nursing care as stigma is attached so strongly to this illness that even some well educated people refuse to serve them. Many are afraid of consulting the doctors as they did not wish other people to know about their predicament. With the existing treatment, people with HIV can lead a normal life particularly if they receive good support from their family members, especially their parents.
The situation is aggravated by the fact that major percentage of the HIV positive individuals are Injectible drug users (IDUs), who are marginalized by society and criminalized by the law. HIV/AIDS has already been concentrated epidemic among the IDUs. They must be taken under rehabilitation to stop the spread of this threat. Conditions of women living with HIV/AIDS are dismal. Women are blamed for carrying the infection, even though they may have got the virus from their partners (in most cases husbands). Instances have been reported, where husbands abandon their ailing wives and children to find another wife. Due to the fear of social and family desertion, women are hesitant to disclose their HIV/AIDS status. Also, disclosure may lead to loss of job and reputations. This fear and dithering will make women an easy target of violence and abuse.
Justification of the study
The Government of Bangladesh estimates that there are 7,500 people living with HIV/AIDS (PLWHAs) in Bangladesh. According to the Joint UN Programme on HIV/AIDS (UNAIDS), this figure is approximately 13,000 people, or less than 0.2 per cent of the adult population (2003). National sero-surveillance in 2005 found a low HIV prevalence (less than 1 per cent) among groups such as female and male sex workers, men who have sex with men, Hijras (transgenders), heroin smokers, and some groups of internal migrants. Nevertheless, HIV prevalence among male injecting drug users (IDUs) in central Bangladesh is rising steadily: at 4.9 per cent, it is close to a concentrated epidemic. Available data indicates that IDUs are well connected to the surrounding community, both sexually and through selling blood, putting the wider population at risk. Young people are also emerging as a key group vulnerable to HIV infection.
PLWHAs in Bangladesh, as in many countries of the world, face manifold socio-economic and cultural problems in society. In the absence of a friendly environment, most of the identified PLWHAs and their family members have to confront stigma, discrimination, and violation of human rights. This situation has also increased the number of invisible PLWHAs, resulting into their non-accessibility to care, counselling and support. Most of these PLWHAs prefer to live without disclosing their status because of fear and shame, or they simply are not aware of the available facilities for care and support. This situation has, however, led a handful of PLWHAs to build contacts among themselves to form their own organisations and network.
As the numbers of people infected with HIV rise, social and economic vulnerabilities are heightened. Population movements (cross border/rural-urban migration and trafficking), unprotected sexual activities and injecting drug use are among the factors that highlight the need to act quickly and effectively. After nearly a decade and a half of the epidemic, facilities for care and support remain inadequate. Stigma and discrimination confront people living with HIV/AIDS (PLWHAs). Lack of awareness and understanding have been obstacles standing in the way of prevention efforts, and inappropriate overtones – condemnation and judgment of infected people – have led to discrimination and even violence against them.
This study will explore the socio-cultural problems faced by PLWHAs and change the attitude and thoughts of the people towards PLWHAs.
Operational Definition
- HIV: Human Immunodeficiency Syndrome. A condition in human in which the immune system begins to fail leading to life threatening opportunistic infection14
- AIDS: Acquired Immunodeficiency Syndrome. A collection of symptoms and infections resulting from the specific damage to immune system caused by HIV virus in human.
- Opportunistic infections: A serious infection with a microorganism which normally has little or no pathogenic activity but which has been activated by a serious disease.
- Epidemic: The unusual occurrence in a community or region of disease. Specific health behavior or event clearly in excess of expected occurrence.
- Discrimination: A practice of treating a particular group in the society less fairly than others.
- Sexually Transmitted Disease (STD): Sexually Transmitted Disease refers to disease of genital organs of either sex transmitted through sexual contact.
- Service: Service is an occupation which includes government and private services.
- Monthly family income:
Upper class- indicates family income is tk.30, 000 per month or more.
Middle class- indicates family income is more than tk.10, 000 but less than
- 30, 000 per month.
Lower class-indicates family income is tk.10, 000 per month or less.
Level of education:
Illiterate- Persons who can not write their name.
Primary level- Persons who write down their name.
Secondary level- Persons who are studied up to class x.
Higher secondary level- Persons who are studied up to class xii.
Tertiary level- Persons who are studied diploma, graduate or post graduate etc.
Research Question
What are the Socio-Cultural Problems faced by People Living With HIV/AIDS (PLWHAs) in Bangladesh?
REVIEW OF RELATED LITERATURE
A study titled ‘People living with HIV stigma index’ conducted on 238 HIV positive people revealed that 16.8 percent of them decided not to go to a hospital when they needed to do so because of the discriminatory attitude of most of the health providers. The study showed that some 84.9 percent of the HIV carriers decided not to have more children because of their uncertain future, while 70 percent of them feel ashamed for their HIV status. The social stigma is so deep-routed in the society that 21 percent PLHIV still believes that they should commit suicide. The recommendations from the study include all HIV prevention interventions should incorporate psycho-social counselling, especially to handle the internal stigma and trauma management. Comprehensive training for the health service providers on stigma and discrimination and its impact on public health management should be addressed, while mass media campaign addressing stigma is also important.
HIV stands for human immunodeficiency virus. This is the virus that causes AIDS. HIV is different from most other viruses because it attacks the immune system. The immune system gives our bodies the ability to fight infections. HIV finds and destroys a type of white blood cell (T cells or CD4 cells) that the immune system must have to fight disease. AIDS stands for acquired immunodeficiency syndrome. AIDS is the final stage of HIV infection. It can take years for a person infected with HIV, even without treatment, to reach this stage. Having AIDS means that the virus has weakened the immune system to the point at which the body has a difficult time fighting infections. When someone has one or more of these infections and a low number of T cells, he or she has AIDS. Scientists identified a type of chimpanzee in West Africa as the source of HIV infection in humans. The virus most likely jumped to humans when humans hunted these chimpanzees for meat and came into contact with their infected blood. Over several years, the virus slowly spread across Africa and later into other parts of the world.
The course of untreated HIV infection can be divided into three phases: the acute HIV disease, then the latency phase and finally the disease of Aids, ending in death. The acute HIV disease lasts a few weeks. This period is also known as the window of vulnerability, and it is characterized by an explosive replication of the HIV. During this phase, the HIVs invade the organs of the defence system and other bodily organs and establish themselves there. The latency phase lasts on average 10 years, during which the virus concentration is relatively low. In the Aids phase the defence system is completely destroyed, as the result of which death occurs after 1-2 years. The defence system (immune system) has two main jobs: as well as combating outside invaders such as bacteria, viruses, fungi etc., which give rise to so-called infectious diseases, it also prevents cancer by tracking down and destroying the body’s own damaged or degenerate cells.
It takes several years before the human immune system is defeated by the HIV infection. A veritable war goes on between the immune system and the viruses, with many battles. As early as a few days after infection (during the acute infection stage) several thousand million new viruses are formed and at the same time thousands of millions of helper cells are destroyed. Hence, 2-3 weeks following infection, the acute HIV infection (= primo-infection) can appear, which subsides again after about 6 weeks, when the human immune system has gained the upper hand in the first battle. Even during the symptom-free latency period, the viruses replicate with extraordinary vigour. The human immune system kills as many HIV as are produced, maintaining equilibrium year upon year. When AIDS itself occurs, the immune system becomes exhausted and the quantity of virus steadily increases. The weakening of the immune system through HIV infection makes people increasingly vulnerable, especially to infectious diseases and cancer.
Diagnosis: HIV can’t be diagnosed through a medical examination or via disease symptoms. Diagnosis is only possible on the detection of the HIV virus or antibodies in body fluids (e.g. blood). Normally the presence of antibodies is tested. The diagnostic window: It takes some weeks before sufficient quantities of antibodies exist in the blood for the test. This period from infection to proof of infection is called the diagnostic window. The period varies from person to person and is dependent on several factors (transmission path, quantity of transferred viruses, immune system etc.). The diagnostic window can be reduced by an average of 3 weeks with the use of an antigen (virus) test or a combination of antigen and antibody tests. For most people the time taken between infection and diagnosis is 3 months but it may take 6 months before it is possible.
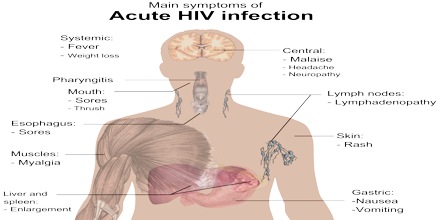
Clinical Stage: The American health authority CDC (Centre for Disease Control and Prevention) defines 3 clinical stages of the disease and 3 immunological categories. According to the CDC definition HIV can only be diagnosed with a confirmed HIV positive test. Stage A covers both the acute HIV illness and the subsequent clinical latency. The acute HIV illness arises 3-6 weeks after infection for 50-70% with flu type symptoms: fever, skin eruptions, throat inflammation, muscular pains, lymph node swelling, headache, and nausea. During clinical latency there are no further complaints although some people have continuous Lymphadenopathie in the shoulders, back or neck. The clinical latency can last for many years. Stage B consists of disease symptoms prior to stage C (AIDS), which further weakens the immune system. Usually these symptoms accompany a general worsening of health. In addition to long lasting (a month plus) symptoms such as fever, night sweats and weight loss, many other infections such as Candida infections of the mouth and throat or viral illnesses like belt rose occur. Stage C is the final phase of the HIV infection, the actual AIDS illness. It is the collapse of the immune system. The pattern of the AIDS illness is unmistakable although individual symptoms may vary. Diverse infections and cancers are common, as are fungal infections of the oesophagus and special forms of pneumonia (Pneumocystis carinii Pneumonia), also common are virus illnesses (i.e. retinal inflammation CMV-Retinitis), parasite infection (i.e. Toxoplasmosis that causes brain abscesses), rare cancer forms (e.g. Kaposisarkom, Lymphdrüsensarkom, brain tumours) as well as neurological illnesses (among other things HIV dementia) and strong weight loss (Wasting syndrome).
Transmission: HIV is passed from person to person: HIV is found in body fluids such as blood, semen, vaginal fluids and breast milk. It is passed from one person to another or transmitted – only in very specific ways. These are:
- Through sexual intercourse between a man and a woman or between two men;
- Through infected blood – for example through contaminated blood transfusions or unsterilized needles and syringes. ( In most places today blood transfusions are completely safe because the blood is tested for HIV before it is used to treat patients); and
- From an infected mother to her baby while it is still in the womb or during childbirth or during breastfeeding.
HIV does not spread through “casual” everyday contact between people. It is not transmitted by coughing, or sneezing, or by touching or hugging someone who has the virus. It is not spread in air, water or in food, or by sharing cups, bowls, cutlery, clothing, or toilet seats. And HIV is not transmitted by biting insects such as mosquitoes, because the quantity of blood on their mouthparts is too minute. HIV can be passed on by infected blood: If blood from a person infected by HIV gets into the blood stream of another person, it will infect them also with the HIV. This can happen: If contaminated instruments are used to pierce the skin during:
- injections
- circumcision
- scarification
- ear piercing
- tattooing
- acupuncture
Infection can be prevented if the equipment used is brand new, or is carefully sterilised each time it is used. From a blood transfusion with infected blood: Blood transfusions may be necessary
- after a bad accident, if someone has lost a lot of blood;
- during a hospital operation;
- after childbirth, if the mother has lost much blood; or
- If a person is anaemic due to bilharzias, hookworm or malaria parasites.
If the blood or equipment used is contaminated with HIV, this will be transmitted to the person receiving the blood, and so they will also become infected. All equipment used for blood transfusions should be sterilised before it is used. In some countries all blood which has been donated is tested for HIV infection, and only non-infected blood is used. More and more countries are now trying to do this. There is no risk in donating blood if the equipment is new or properly sterilised.
In addition to the risk of infection from sexual contact, HIV can be transmitted through transfusion with HIV-infected blood or blood products, or from a needle stick injury involving a needle used by an HIV-infected person. The most common form of transmission of HIV by needles occurs when persons using illegal injecting drugs share needles. It is also possible to become infected when infected blood, or a bodily fluid containing infected blood, comes in contact with mucous membranes or skin that is broken or open. Universal precautions have been recommended for anyone who might come in contact with blood or body fluids. These precautions apply also to body fluids that contain blood and to certain body fluids that are not generally found outside the body, for example, vaginal secretions, semen, and cerebrospinal fluid. Bodily fluids to which universal precautions do not apply (unless blood is present in them) include faeces, tears, sputum, saliva, nasal secretions, vomits, and urine. However, these fluids can contribute to the spread of infections other than HIV, so some precautions should be taken in handling them.
Testing: If someone has been at risk of contracting HIV, testing is the only way to find out whether or not they have become infected. The test should be combined with comprehensive counselling by a doctor. The HIV infection has, within the space of only a few years, developed into a pandemic (worldwide epidemic). It is, therefore, important for all persons to know whether they are infected or not, since in this way each one of us can contribute towards preventing the further spreading of this fatal disease. Deceptive calm: As a rule an infected person notices nothing (with the exception of an occasionally occurring influenza-like illness within the first weeks) of the HIV infection for several years – a deceptive calm. In this symptom-free period, which lasts on average ten to twelve years, the infected person is already a transmitter of the disease. Whether one has become infected or not can only be ascertained by making an HIV test. Those who have themselves tested are behaving responsibly both towards themselves and towards others.
The test always makes sense: Let us assume that the person in question is not infected at all, i.e. HIV negative. The negative test result indicates the absence of an infection with a high degree of certainty – provided that the recommended waiting period before the test has been observed (see below). Any uncertainty and any unnecessary fears can now be assuaged. In this situation, combined with competent counselling, a responsible pattern of behaviour (with avoidance of risk situations) can be developed for the future. Let us assume, on the other hand, that someone is infected, i.e. HIV positive. This person will, as a rule, do everything possible not to spread the disease further. No-one would like to infect his/her partner, the person he/she loves most, or cause the birth of an HIV positive child. On the other hand only those persons can profit from timely therapy (which can postpone the terminal stage AIDS), who know that they are HIV positive. In many of the complications accompanying AIDS, early recognition plays an important role. Such manifestations can be treated in time, and much suffering can be prevented. An HIV positive person who places him/herself under competent medical care, can live longer and better than someone who delays until the onset of AIDS.
The test performed by a doctor in whom you have confidence, so that comprehensive counselling can follow. Treat immediately and correctly: When an HIV positive person falls victim to other infections, this contributes to the proliferation of the virus, and thus to further weakening of the immune system. Basically harmless diseases – e.g. shingles – can take a very severe course. Many diseases, e.g. diarrhoea, must therefore be treated at an early stage. It is essential for a doctor to know whether his patient is HIV positive or not. Only then can he make a correct diagnosis and initiate correspondingly effective therapy. For example in the most frequent type of pneumonia encountered in HIV positive patients, Pneumocystis-Carinii-Pneumonia (PCP) completely different drugs have to be employed than in “normal” pneumonia. At the time when PCP was treated as normal pneumonia almost half of the patients died. But now, with early diagnosis and appropriate therapy, less than five per cent of these patients die.
In patients known to be HIV positive a virus disease of the eyes (CMV Retinitis), which frequently occurs in AIDS patients, can be diagnosed at an early stage and treated, preventing them from going blind. Anyone who keeps putting off the decision to submit him/herself to an HIV test, will, if infection is present, lose valuable treatment time. There are also other reasons why a test should be made: in the case of certain inoculations, e.g. before travelling overseas, the doctor has to adopt a different procedure in the presence of an HIV infection to ensure that the patient comes to no further harm. The same applies to major operations which, as everyone knows, represent an exceptional strain on the immune system. In the interest of the patient the nature of the operation must be considered very carefully.
Medical advice: Only if HIV positive individuals know that they are infected can they take specific precautions to safeguard their health. How many people are aware that birds in the apartment can, with their excrement, because dangerous fungal diseases in HIV infected persons, or that cat toilets and the soil in flower pots can hold similar risks? Alcohol, cigarettes and drugs are even more harmful for HIV positive persons, since they weaken the immune system additionally. Raw meat and other foodstuffs likely to be contaminated with salmonella should be strictly avoided, as should raw fish, oysters and other sea foods. Mayonnaise and sauce or gravy that have been left standing too long can also be dangerous. In contrast, healthy nutrition rich in calories and vitamins is to be recommended. Contacts with carriers of pathogens (germs) – whether children’s’ diseases (e.g. chicken pox) or tuberculosis – can become dangerous. Travelling to countries with a low standard of hygiene – above all tropical countries – may involve above-average dangers of infection. The taking of medicines without first consulting the doctor should be avoided due to possible side effects or weakening of the immune system. And, what many people do not know, severe physical strain or stress, as well as sun-bathing in the open air or in the solarium, can also affect the immune system, and thus accelerate the outbreak of AIDS. In the interests of all infected persons, all the points mentioned speak in favour of an HIV test. But there is also a further reason: for several years now the medical world has been in possession of virus-inhibiting medications.
When a test should be made:
- In the event of a previous way of life involving risk (e.g. drug dependence or frequent change of partners)
- Both partners at the beginning of a sexual relationship
- Partners wanting a child
- Women at the beginning of a pregnancy
- Before inoculation with living vaccines
- If blood transfusions were received before autumn 1985
- Prior to major operations
The test should be taken at the earliest two to six weeks after a possible infection and, in the event of a negative result, repeated after three months. The test no longer makes sense for persons who already know that they are infected.
Antiretroviral therapy (ART): The current therapy for HIV infection is called HAART (Highly Active Antiretroviral Therapy) and consists of a combination of at least three different active ingredients. There are more than 20 different drugs in use. A successful HAART suppresses the viral load (concentration of HIV in the blood) below the detection threshold and indirectly increases the number of T-helper cells. Due to these drugs, an HIV infection changes from a fatal illness into a chronic illness. This way it is possible to prevent the appearance of symptoms, and also to significantly reduce the risk of infection. The drugs all prevent replication of HIV via various mechanisms, by interrupting the replication cycle. However, these drugs can only work over the long term, if they are taken daily, 365 days a year. Thanks to antiretroviral therapy (ART), people infected with HIV are living significantly longer and have a better quality of life. But ART cannot completely eliminate the HIV in a person and it is not a cure. The drugs must be taken for a lifetime, which is a heavy burden on the patient. As soon as the drugs are stopped, the viruses replicate again explosively. Sometimes the drugs are not tolerated or the HIVs are resistant to these drugs, which therefore do not work any longer.
Currently, the drugs available to combat HIV infection are the reverse transcriptase inhibitors and the protease inhibitors. The reverse transcriptase inhibitors indirectly prevent the viral genome from becoming incorporated in the DNA of the human host cell, as these drugs block an important enzyme for DNA synthesis – reverse transcriptase. The protease inhibitors block protease, a central enzyme responsible for forming new viruses. Nowadays the two types of drug are used in combination. Both help to keep down the level of virus in the blood and lymph nodes and in this way they slow down the progress of the disease. Huge advances have been achieved in the treatment of HIV infection in the last few years. In the early nineties, antiviral therapy was used only in the advanced stages of HIV infection. Nowadays treatment is begun early in the hope: (1) of stopping further proliferation of the virus and destruction of the immune system, thus halting the progress of the disease; (2) of suppressing the formation of resistant HIV variants; (3) of reducing proneness to infection. Studies have shown that in HIV-positive pregnant women, the risk of transmitting the virus to the baby can be greatly reduced by use of antiviral therapy. Nowadays therapy is begun with two different reverse transcriptase inhibitors and one protease inhibitor. Reverse transcriptase inhibitors include AZT (Retrovir®), Lamivudin (3TC®), ddI (Videx®) or ddC (Hivid®). Protease inhibitors are Indinavir (Crixavan®) or Nelfinavir (Viracept®).
Drugs for Prophylaxis in cases of AIDS: Prophylaxis is aimed at preventing or at least delaying onset of typical infections (opportunistic infections) in the AIDS stage. It only combats the symptoms and does not cure the HIV infection, nor is it a way of halting the destruction of the immune system. The precise procedure for prophylaxis against opportunistic infections depends on the stage of the disease. Various drugs are used: e.g. Baktrim® for prophylaxis against Pneumocystis carinii pneumonia. Post-exposure prophylaxis (b) For several years now, medical and nursing staff exposed to the risk of HIV infection by an injury at work – from a used syringe, for example – have been treated for two to four weeks with one or more anti-HIV drugs. This has reduced the risk of transmission by 80%. Since 1997 this “treatment” has been available in Switzerland also to persons who may have become infected through unprotected sexual contact with an HIV positive partner. But little is known at present about the effectiveness of the “treatment”, except that it should be started as soon as possible, ideally within a few hours, but not later than 72 hours after the infection risk situation, otherwise the HIV will already have spread in the body. These drugs must be taken for two to four weeks and have strong side-effects. The decision to carry out PEP needs careful consideration by a doctor in a central hospital, as nothing is yet known about long-term damage through antiretroviral therapy on healthy individuals.
What you one know about the test: The test used to ascertain whether someone has become infected with the AIDS Virus, HIV, is called the HIV antibody test (e.g. the ELISA). What is looked for is not the virus itself, but the products of the human defence system (immune system) in the blood, i.e. the antibodies. The HIV test is one of the surest tests in medicine. The time from the moment of infection until the appearance of antibodies in the blood (seroconversion time, diagnostic window) varies, and is dependent on various factors (route of transmission, number of virus particles transmitted, etc.). As far as we know today, antibodies appear at the earliest after two to six weeks and, in the majority of people within three months, and therefore testing are effective at the earliest two to six weeks after exposure to risk of infection. If the result is then negative, the test should be repeated 3 months later.
There are various tests, and these complement each other. The ELISA is used as an HIV antibody detection test. Since other antibodies may also interact, “positive” results are always rechecked. For confirmation or correction the Western Blot Test is used. It is more time-consuming and expensive than the more sensitive ELISA. To exclude possible sample switches in the laboratory, in the event of a “positive” result a second blood sample is to be recommended. Antigen tests, which demonstrate viral components directly, are less sensitive than the HIV antibody test, and give no essential shortening of the diagnostic window. The antigen test is important in identifying those newly infected with HIV. The PCR test (gene probes, with which even traces of genetic material of the virus can be detected) is, because of its complexity, used only by specialists and when test results are unclear e.g. in early diagnosis in infants and uncertain cases of infection with HIV. The PCR Test is nowadays used to measure the effectiveness of therapy.
Only people who are aware of their infection can behave responsibly towards themselves and others.
- Infected persons should, in principle, inform all previous sexual partners about the existence of the infection, so that they can also have themselves tested at once and receive medical counselling. In this way can it be ensured that they profit at an early stage from the medications available today, and that they do not unwittingly transmit the infection further
- Infected persons must inform their present sexual partner about the infection. Safe protection means abstaining from sexual intercourse and the exchange of body fluids. Condoms reduce the risk of infection, but they do not exclude it completely. Someone who does not want to change his/her risky pattern of behaviour should always protect him/herself with condoms.
- In sexual intercourse between infected persons it is worthwhile using condoms to reduce the risk of infection with other pathogenic organisms (syphilis, herpes, hepatitis etc.) or with a particularly “virulent” HIV strain.
- Infected persons must inform doctors, dentists and nursing staff about the infection, so that the latter can act accordingly.
- Blood, organ and sperm donations from infected persons are forbidden.
All the points set out here ought to be obvious as ground rules of caring and considerate behaviour.
Injecting drug users, sex workers and men having sex with men are considered most at-risk groups to HIV infection in Bangladesh. Between 20,000 – 40,000 people in Bangladesh inject drugs, 57% borrow needles and only one in three used sterile equipment. This percentage is much higher in female injecting drug users (74%). More than half (57%) of injecting drug users (IDUs) are married and most IDUs are sexually active (with an average of two partners). In Dhaka, the HIV rate among IDUs is 6.4%5. Commercial sex work occurs in Bangladesh as it does in other Asian countries. Most married men who have unprotected sex with sex workers continue to have unprotected sex with their wives, exposing them to infection with HIV and other sexually transmitted diseases. Low condom use, risky behaviour and general lack of understanding about HIV is not limited to clients of sex workers. In fact these traits are widespread and heighten the chances of a HIV epidemic in Bangladesh. Although many people have heard of HIV, their knowledge is limited in regards to how it is transmitted and how they can protect themselves. Nearly one in five ever-married women who had heard of AIDS did not know if there was any way to prevent it. This was lower for men, at 6%6. Men having sex with men are largely hidden due to the powerful stigma and discrimination they face in Bangladesh. Many men who have sex with men are bi-sexual and do not necessarily identify themselves as such. Men buying sex from other men rarely use condoms and many continue to have sex with their wives20.
Migrant workers are another important group identified as a priority in the Bangladesh National Strategic Plan for HIV and AIDS 2005-2010. Approximately 250,000 people leave Bangladesh for employment every year. The risk is that they will get infected during their stay abroad and return to Bangladesh where they may transmit the virus to others especially their wives who could in turn transmit infection to their babies. Migrant workers account for a significant number of HIV cases in Bangladesh, primarily because they are subjected to mandatory HIV testing. According to the International Centre for Diarrhoeal Disease Research (ICDDR), 47 of the 259 cases of people living with HIV between 2002-2004 were infected as a result of migration. Of these, 29 were males returning from abroad, seven were wives of migrant workers, and four were children of HIV positive migrant workers. In 2004, data from the National AIDS/STD (Sexually Transmitted Disease) Programme showed that 57 of the 102 newly reported HIV cases were among returning migrants. According to the recent Children and AIDS, Third Stocktaking Report 2008 published by four UN agencies, only 16% of girls aged between 15 and 24 have a comprehensive knowledge of HIV in Bangladesh. There is a high level of misconception among youth. More than half believe that HIV/AIDS can be spread by coughing or sneezing and 50% believe that HIV can be spread through sharing food or water with a HIV infected person.
Although young Bangladeshis are at risk of HIV very few believe so – 22% of unmarried males reported having premarital sex, almost 60% of whom had never used condoms. This has impacted on the rate of STIs; almost one in five men, and two in five adolescent boys, reported having at least one symptom of a sexually transmitted infection (STI) in a 2004 health survey. Women also require special attention in HIV interventions in Bangladesh, given their social, economic and political status. Women are four times more likely to contract HIV than men.
Women’s lower social and cultural status also causes them to have less access to education, employment opportunities and health care, including opportunities for HIV tests, counselling and medical care. Women are often subjected to early marriage, sexual abuse and violence in intimate and marital relationships. An increasing number of women are forced to sell their bodies as the only way to survive and provide for their children. Men who buy sex from women are often reluctant to use condoms. Because women have little negotiating power, even within their marriages, they may have unprotected sex with their spouses who might be engaging in one or more high-risk behaviours and be exposed to HIV.
The HIV prevalence among the general public is not fully known; currently available surveillance data only covers high risk groups. This ambiguity is partly because voluntary and confidential counselling and testing (VCT) services are not widely available in Bangladesh. While HIV tests are available in some private health settings, in many cases there is no counselling support and no confidentiality guarantee. Many HIV positive people tested both in private and government facilities have seen their names and other personal details published in the local or national media. Social values, lack of adequate information, the stigma attached to HIV and AIDS, and the lack of confidentiality are not conducive for people, especially the younger population, to seek out HIV tests.
All of these factors are compounded by unsafe blood transfusions and the reuse of injection syringes; an increased rate of external and internal migration by people seeking work or a better economic environment; and the fear, stigma and secrecy attached to STIs.
HIV positive people are ignored in the society in Bangladesh. There are a lot of cultural stigma and misconception about them. Positive people have been treated generally as a criminal. They are isolated from the society, family and friends. But they have all rights to live as a normal citizen of the country. The positive person can come in the open and speak in their own voice and play active role in making the problem visible to the policymakers, care givers, media people, staff of DHARA and the general people. If we could ensure it and break their silence, life of the PLWHAs would be changed dramatically.
Stigma and discrimination: Stigma and discrimination is widespread over the region. Bangladesh. Lack PLWHA networks, and still have to overcome a deep-rooted stigma before PLWHA feel secure enough to step forward. In Bangladesh there are examples of HIV positive people being thrown into jail or isolated lockups. Eight positive people have got together in Dhaka and are trying to form a network of PLWHAs. There are numerous incidents across the region of rejection of PLWHAs by doctors and paramedical staff and refusal to requests for treatment. This can be attributed to the fear of contracting the infection from PLWHAs, especially in places that do not have the facilities to enable the doctors to practice universal precautions. Just getting rid of irrational fears of infection by the dissemination of information is not going to reduce discrimination and stigma, if these originate from reasons other than lack of information, the voices of HIV positive people are rarely heard and their faces seldom seen in pubic. People living with HIV/AIDS cannot come out and live positive lives without fear of having their future shattered in light of the pervasive climate of denial, stigma and discrimination that exists. This lack of an enabling environment seriously jeopardises the efforts to bring a halt to the epidemic and mitigate its human, social and economic costs.
Legislative measures to protect vulnerable groups Groups targeted by NASP are susceptible to police excesses, because criminal laws are in direct conflict with HIV policies. So far, no legislative measures have been adopted to repeal these laws and protect the interests of the vulnerable population. Stigma, discrimination and denial Stigma continues to be a major barrier to working with HIV-positive people. A major cause of stigma is the association of HIV with sexual promiscuity and immoral behaviour. Awareness-raising programmes tend to focus on how HIV is spread; there is very limited discussion on human rights and AIDS, discrimination and stigma issues. There are very few education programmes among the medical community. As a result, public perceptions of PLWHAs and members of vulnerable populations are very negative. Incidences of stigma and discrimination against PLWHAs by the medical community are also common, which prevents a large section of PLWHAs from accessing public or private health services.
Socioeconomic and social – cultural factors: Unfortunately, a low level of awareness on HIV/AIDS still prevails among the general population as well as the high-risk behaviour groups. The 1999-2000 Bangladesh Demographic and Health Survey found that over 90% of rickshaw pullers could not identify a single correct method of HIV prevention. Only 31% of married women and 50% of currently married men had heard of HIV/AIDS. Yet, in a survey on premarital intercourse, Population council found that 29% of women nineteen years and older and 69% of married men in rural and urban areas had engaged in premarital intercourse. In a population based study of 1541 slum dwellers the mean age at first sexual intercourse for men was 19 and for women was 14.75 years. In in-depth interviews with 120 of these respondents, most women reported their partners to be their husbands, while most men reported their premarital partners to be CSWs, women who they pretend to love, women who they did love, and 8.5 % of the 540 male survey respondents reported male sexual partners. The evidence is mixed as whether there is a class differential in premarital sexuality. One study found the incidence of premarital sex to be higher in the lower socioeconomic class than in the higher class. However, a 1997 Population Council survey reported no major differences between the people living in poor or well-off areas.
Based on this information, we see that the ongoing efforts in Bangladesh require a paradigm shift from a health response to addressing HIV/AIDS as a human development issue. This requires action to deal with the socioeconomic and cultural factors that render individuals and communities vulnerable to HIV/AIDS
Availability and accessibility of services: Issues related to care cannot be dealt with in isolation. Some of the issues touched upon here are as much a part of Stigma & Discrimination or Human Rights. In theory no government in the region has denied that people living with HIV/AIDS also deserve health care – and that their need for this is often more acute than that of others. But the reality is that PLWHAs are often denied access to necessary health services, all over the region. In some countries, there is such complete denial that there is no expectation from PLWHAs of receiving any medial support.
Human Rights: In Bangladesh the situation of human rights in relation to PLWHA seems critical. As PLWHAs are not visible, the reality of the human right situation is difficult to estimate. To Human Rights Watch, “People living with HIV/AIDS and those thought to be infected have been imprisoned, assaulted and even murdered. The stigma of AIDS has taken many lives before the disease itself killed them. But the reasons behind the suicides and extent of this have rarely come to our knowledge. Society’s limited understanding of this disease is causing innocent people to pay a terrible price. Increasingly across the world, there are voices questioning in one angle. They question the narrow approach to a single disease, especially the huge financing for AIDS over all else in basic health care. Our approach to this disease needs to change for the sake of our people, our brothers and our sisters who are fighting against odds.
Social factors like discrimination, stigmatization and rejection have pushed people living with HIV to become desperate and feel hopeless, to the extent of giving up their life. They face discrimination and lack of support not only from the society but also from his/ her own family. They are also being confined from friends, scared for losing their jobs. This made them to live in phobia and their condition become worse as they need proper and adequate treatment that could provide them with better life. Most of these people are not getting proper medical and nursing care as stigma is attached so strongly to this illness that even some well educated people refuse to serve them. Many are afraid of consulting the doctors as they did not wish other people to know about their predicament. With the existing treatment, people with HIV can lead a normal life particularly if they receive good support from their family members, especially their parents.
The situation is aggravated by the fact that major percentage of the HIV positive individuals are Injectable drug users (IDUs), who are marginalized by society and criminalized by the law. HIV/AIDS has already been concentrated epidemic among the IDUs. They must be taken under rehabilitation to stop the spread of this threat. Conditions of women living with HIV/AIDS are dismal. Women are blamed for carrying the infection, even though they may have got the virus from their partners (in most cases husbands). Instances have been reported, where husbands abandon their ailing wives and children to find another wife. Due to the fear of social and family desertion, women are hesitant to disclose their HIV/AIDS status. Also, disclosure may lead to loss of job and reputations. This fear and dithering will make women an easy target of violence and abuse.
Level of Involvement of PLWHAs: It has been found that there is an absence of effective involvement of PLWHAs at every level of the initiatives against HIV/AIDS throughout the region. PLWHAs have to be included at all levels of programme planning and implementation. Their views have to be solicited from the initial stages of the dialogue and they have to be included in the team that plans the objectives and activities. Including them in the monitoring and evaluation is also essential. PLWHAs are unique in possessing a special insight in and commitment to the success of the programmes. Moreover, since there are a number of organisations, especially NGOs, which have PLWHAs working for them, there is a pool of PLWHAs who possess the know-how of planning, implementation, monitoring and evaluation, and others with the potential to learn the same. It has been demonstrated by smaller efforts such as Counselling Centres, Care Homes, etc that clients respond best to fellow PLWHA, thereby increasing the chances of the programme’s success. Another way of involving the PLWHAs and building their capacity is for all organisations working in this field to employ PLWHAs and include them in all their activities.
Networking: The total number of PLWHAs who are known to have disclosed their status is not more. Of them one positive woman committed suicide recently. The PLWHAs have no registered organisation in Bangladesh. Nevertheless there is an initiative to form a self help group of people living with HIV/AIDS under the name of Ashar Alo (Light of Hope). The group wants to get their organisation registered with the appropriate government ministry. With support from a group of NGOs another initiative has been taken by positive people who formed a National Network of PLWHAs in Bangladesh on 20 January 2001 Taking stock of their situation, they have developed objectives for their network, as below.
Objectives of the National Network of PLWHAs in Bangladesh
- To protect the rights of PLWHAs.
- To establish and enhance contact with support organisations and national, regional and international networks.
- To ensure participation in policy making and implementation of the HIV/AIDS programme at national level.
- To co-operate with the government and non governmental organisations in their HIV/AIDS prevention programmes.
- To provide necessary information, counselling and services to HIV positive people.
The PLWHAs and their organisation/network, most of them had never heard of the Paris Declaration. Nevertheless, their activities aimed at reaching the goal of “greater involvement” in response to the HIV/AIDS situation in the country with the effective assistance of the NGO Support Network. PLWHAs Network and supportive NGOS would be a first step in increasing the influence of PLWHA. The PLWHAs expressed the need for skills to advocate for their concerns at various local, national and regional forums. All agreed that to respond to the HIV/AIDS epidemic in Bangladesh, it would be necessary to involve PLWHAs and other marginalised communities in policy and programme development, implementation and evaluation, management and administration. The PLWHAs organisations and individuals would also have critical contributions to make in the creation of a supportive environment for all HIV positive people in society.
Study Objectives
General objective
- To explore the Socio-Cultural Problems faced by People Living With HIV/AIDS (PLWHAs) in Bangladesh.
Specific objectives
- To describe the socio demographic factors associated with the Socio-cultural problems faced by PLWHAs in Bangladesh.
- To explore the level of knowledge related to HIV/AIDS in relation to the Socio – cultural problems faced by PLWHAs in Bangladesh.
- To asses the mode of transmission of HIV/AIDS to identify the Socio-cultural problems faced by PLWHAs in Bangladesh.
- To demonstrate the behavioural pattern faced by PLWHAs from their family and society to identify the Socio-cultural problems faced by PLWHAs in Bangladesh.
- To asses the access to media for information and treatment of PLWHAs in relation to the Socio-cultural problems faced by PLWHAs in Bangladesh.
Study Design:
My study design was a Descriptive Cross Sectional Study.
Study Population: People Living With HIV/AIDS in Bangladesh
Study Area:
Organizations dealing with PLWHAs:
| Ashar Alo, C/o CCDB (Christian Commission for Development in Bangladesh), 88, Senpara Parbatta, Mirpur-10, Dhaka-1216. | CARE Bangladesh, House No. 66, Road 7/A, Dhanmondi, Dhaka-1209, GPO Box-226 |
| CAAP (Confidential Approach to AIDS Prevention), House no 63, Block-D, Road 15, Banani, Dhaka-1213. | CCDB (Christian Commission for Development in Bangladesh), 88, Senpara Parbatta, Mirpur-10, Dhaka-1216 |
| HASAB ( HIV/AIDS&STD Alliance Bangladesh), 4/1, Iqbal Road,Mohammedpur,Dhaka- 1207 | SHISHUK(Shishuk Shastha Unnayan Karzkaram), 7/1,Block-A, Lalmatia, Dhaka-1207 |
| IDHRB (Institutional Development of Human Rights in Bangladesh), House No. 500/h, Road 8, Dhanmondi R/A, Dhaka-1205 | Rotary Club Dhaka , 168/C, Green Road, Dhanmondi, Dhaka- 1205 |
Study Period:
My study was carried out from November 2010-February 2011.
Sample size:
Due to minimum number of AIDS patients identified in our country and from them limited patients are corresponding with the organizations dealing with People Living with HIV/AIDS (PLWHAs) therefore, my sampling technique was purposive and my sample size was dependent on patients available in the organizations. My sample size was 100.
Inclusion criteria
- The study was conducted with only PLWHAs.
- The study was conducted only PLWHAs with the mentioned organizations.
- People who were normal in sense and able to provide information.
Exclusion criteria
- People who were unable to give information.
- People who refused to give consent.
- People who were absent in interview time.
Sampling technique:
Sample was selected purposively considering the inclusion and exclusion criteria.
Data collection tools and technique
There were the following data collection procedures.
- A semi structured questionnaire was designed and pre-tested to collect the information on socio-demographic, Socio-economic, knowledge and attitude related factors.
- Focus Group Discussion (FGD).
Data management and Analysis plan:
After collection of data, this was checked and verified for consistency and reduction of errors. Thereafter these data was transferred to a suitable master sheet for processing and subsequent analysis. Data was entered to the computer and saved in Statistical Package for Social Sciences (SPSS) ver 16.00 by the Research. Quality and reliability of collected data were re-checked. Appropriate statistical analysis, calculation and test were carried out to relate variable according to the objectives of the study.
Ethical considerations
- Right to refuse and withdraw from the study at any time was accepted.
- Respondent was told that the collected data from the interview would be kept confidential and would be used for the study purpose only.
- All interviews were conducted with the prior consent of the respondents.
- No incentives would be given to the respondents.
RESULTS
This was a descriptive cross sectional study conducted among the HIV/AIDS patients in Dhaka City. Samples from November 2010 to February 2011 was taken and studied. All data were taken, managed and analyzed.
Table: Distribution of the respondents by their age (n=100)
| Age | Frequency | Percent |
| Up to 20 years | 25 | 25 |
| 21 years-30 years | 35 | 35 |
| 31years -40 years | 25 | 25 |
| above 40 years | 15 | 15 |
| Total | 100 | 100 |
Table indicates that out of 100 HIV/AIDS patients 25% were up to 20 years of age, 35% were age of between 21-30 years , 25% were aged between 31-40 years, 15% were aged above 40 years.
Table: 2 Distribution of the respondents by their sex (n=100)
| Sex | Frequency | Percent |
| Male | 60 | 60 |
| Female | 40 | 40 |
| Total | 100 | 100 |
Table 2 indicates that out of 100 HIV/AIDS patients 60% were male and 40% were female.
Table: 3 Distribution of the respondents by their occupation (n=100)
| Occupation | Frequency | Percent |
| NGO worker | 38 | 38 |
| Service | 20 | 20 |
| Unemployed | 13 | 13 |
| Students | 10 | 10 |
| Others | 9 | 9 |
| Housewife | 10 | 10 |
| Total | 100 | 100 |
Table 3 indicates that out of 100 respondents 38% were NGO workers, 20% did service, 13% were unemployed, 10% were students, 10% were housewife and 9% did other types of work.
Table: 4 Distribution of the respondents by their marital status (n=100)
| Marital Status | Frequency | Percent |
| Unmarried | 33 | 33 |
| Married | 27 | 27 |
| Divorced | 22 | 22 |
| Separated | 13 | 13 |
| Others | 5 | 5 |
| Total | 100 | 100 |
Table 4 indicates that out of 100 respondents 33% were unmarried, 27% were married, 22% were divorced, 13% were separated and rest 5% had others status.
Table: 5 Distribution of the respondents by route of transmission of HIV (n=100)
| Route of transmission | Frequency | Percent |
| Sexual transmission | 22 | 22 |
| Blood transmission | 27 | 27 |
| Mother to baby transmission | 20 | 20 |
| Do not know | 31 | 31 |
| Total | 100 | 100 |
Table 5 indicates that out of 100 respondents 22% thought their route of transmission of HIV was sexual, 27% thought it was due to blood transfusion, 20% thought for their mother and rest 31% did not know how they got HIV.
Table: 6 Distribution of the respondents by their knowledge on HIV/AIDS (n=100)
| Knowledge on HIV/AIDS | Frequency | Percent |
| Yes | 67 | 67 |
| No | 33 | 33 |
| Total | 100 | 100 |
Table 6 indicates that out of 100 respondents 67% had knowledge on HIV/AIDS and rest 33% did not have knowledge on that.
Table: 7 Distribution of the respondents by their knowledge on VCT and ART (n=100)
| Knowledge on VCT and ART | Frequency | Percent |
| Yes | 57 | 57 |
| No | 43 | 43 |
| Total | 100 | 100 |
Table 7 indicates that out of 100 respondents 57% had knowledge on Voluntary Counselling and testing (VCT) and Antiretroviral Therapy (ART) but 43% did not have idea on it.
Table: 8 Distribution of the respondents living with their family (n=100)
| Living with family | Frequency | Percent |
| Yes | 33 | 33 |
| No | 67 | 67 |
| Total | 100 | 100 |
Table 8 indicates that out of 100 respondents 33% HIV patients were living with their family and 67% were not living with their family.
Table: 9 Distribution of the respondents leaved by their family because of HIV positive (n=100)
| Leaved from family | Frequency | Percent |
| Yes | 44 | 44 |
| No | 56 | 56 |
| Total | 100 | 100 |
Table 9 indicates that out of 100 respondents who were not living with their family 44% were leaved by their family because of their HIV status and 56% respondent’s family did not do that.
Table: 10 Distribution of the respondents facing stigma and discrimination because of HIV positive (n=100)
| Stigma and discrimination | Frequency | Percent |
| Yes | 82 | 82 |
| No | 18 | 18 |
| Total | 100 | 100 |
Table 10 indicates that out of 100 respondents 82% faced stigma and discrimination because of their HIV status and 18% of them did not face stigma and discrimination.
Table: 11 Distribution of the respondents facing verbal abuse by the people (n=100)
| Verbal abuse | Frequency | Percent |
| Yes | 80 | 80 |
| No | 20 | 20 |
| Total | 100 | 100 |
Table 11 indicates that out of 100 respondents 80% faced verbal abuse and because of their HIV status and 20% of them did not face such.
Table: 12 Distribution of the respondents facing physical abuse by the people (n=100)
| Physical abuse | Frequency | Percent |
| Yes | 33 | 33 |
| No | 68 | 68 |
| Total | 100 | 100 |
Table 12 indicates that out of 100 respondents 33% faced physical abuse and because of their HIV status and 68% of them did not face such.
Table: 13 Distribution of the respondent of getting fairly treatment by the health care provider (n=100)
| Treated fairly by health care provider | Frequency | Percent |
| Yes | 72 | 72 |
| No | 28 | 28 |
| Total | 100 | 100 |
Table 13 indicates that out of 100respondents 72% of them were treated fairly by the health care provider and 28% did not get fairly treatment by the health care providers.
Table: 14 Distribution of the respondent by their opinion of disclosing of their HIV status (n=100)
| Agree of disclosing HIV status | Frequency | Percent |
| Yes | 22 | 22 |
| No | 78 | 78 |
| Total | 100 | 100 |
Table 14 indicates that out of 100 respondents 22% of them thought that they should disclose their HIV status and 78% respondents thought they should not disclose their HIV positive status.
DISCUSSION
“Socio-Cultural Problems faced by People Living With HIV/AIDS (PLWHAs) in Bangladesh” was a descriptive cross sectional study. The study population was 100 HIV/AIDS patients who were seeking treatment from selected NGOs in Dhaka City.
It was found that out of 100 HIV/AIDS patients 25% were up to 20 years of age, 35% were age of between 21-30 years, 25% were aged between 31-40 years, and 15% were aged above 40 years. Among 100 respondents 60% were male and 40% were female. Out of 100 respondents 38% were NGO workers, 20% did service, 13% were unemployed, 10% were students, 10% were housewife and 9% did other types of work. In case of marital status of the respondents 33% were unmarried, 27% were married, 22% were divorced, 13% were separated and rest 5% had others status. Among all the respondents 22% thought their route of transmission of HIV was sexual, 27% thought it was due to blood transfusion, 20% thought for their mother and rest 31% did not know how they got HIV. Though all the respondents were seeking treatment from different NGOs in Dhaka City but still they did not have clear idea and knowledge on HIV/AIDS. Among 100 respondents 67% had knowledge on HIV/AIDS and rest 33% did not have knowledge on that.
It was revealed that out of 100 respondents 57% had knowledge on Voluntary Counselling and testing (VCT) and Antiretroviral Therapy (ART) but 43% did not have idea on it. Among all (n=100) 33% HIV patients were living with their family and 67% were not living with their family. We found that 67%( 67) respondents were not living with their family and among that 100 respondents 44% were leaved by their family because of their HIV status and 56% respondent’s family did not do that.
The study identified that out of 100 respondents 82% faced stigma and discrimination because of their HIV status and 18% of them did not face stigma and discrimination. Among all 33% faced physical abuse and because of their HIV status and 68% of them did not face such, and out of 100respondents 80% faced verbal abuse and because of their HIV status and 20% of them did not face such. 72% of the total respondents were treated fairly by the health care provider and 28% did not get fairly treatment by the health care providers. Out of 100 respondents 22% thought that they should disclose their HIV status and 78% respondents thought they should not disclose their HIV positive status.
CONCLUSION AND RECOMMENDATION
HIV-related stigma and discrimination severely hamper efforts to effectively fight the HIV and AIDS epidemic. Fear of discrimination often prevents people from seeking treatment for AIDS or from admitting their HIV status publicly. People with (or suspected of having) HIV may be turned away from healthcare services and employment, or refused entry to a foreign country. In some cases, they may be forced from home by their families and rejected by their friends and colleagues. The stigma attached to HIV/AIDS can extend to the next generation, placing an emotional burden on those left behind.
Today, HIV/AIDS threatens the welfare and wellbeing of people throughout the world. At the end of the 2008, 33 million people were living with HIV with two million having died from AIDS-related illness that year. Combating stigma and discrimination against people who are affected by HIV/AIDS is a vital ingredient for preventing and controlling the global epidemic.
No policy or laws can alone combat HIV/AIDS related discrimination. Stigma and discrimination will continue to exist so long as societies as a whole have a poor understanding of HIV and AIDS and the pain and suffering caused by negative attitudes and discriminatory practices. The fear and prejudice that lie at the core of the HIV/AIDS discrimination need to be tackled at the community and national levels, with AIDS education playing a crucial role. A more enabling environment needs to be created to increase the visibility of people with HIV/AIDS as a ‘normal’ part of any society. The presence of treatment makes this task easier; where there is hope, people are less afraid of AIDS; they are more willing to be tested for HIV, to disclose their status, and to seek care if necessary. In the future, the task is to confront the fear-based messages and biased social attitudes, in order to reduce the discrimination and stigma of people living with HIV and AIDS.
APPENDIX-A
Investigator’s signature & Date
Volunteer’s signature/Thumb
impression & Date
Witness signature/ Thumb impression & Date
APPENDIX – B
Socio-Cultural Problems faced by PLWHAs in Bangladesh
Questionnaire
Name of the respondent (Optional):
- Age (Full in year)
- Gender
- Male
- Female
- Occupation
- Service
- Business
- Student
- House wife
- Commercial sex worker
- Track drivers, Rickshaw pullers
- Monthly family income:
- Upper class
- Middle class
- Lower class
- What is your religion?
- Islam
- Hinduism
- Christianity
- Buddhism
- Other
- Level of education :
- Illiterate
- Primary level
- Secondary level
- Higher secondary level
- Tertiary level
- Marital status:
- Unmarried
- Married
- Widow
- Separated
- Other (Please specify)
- of Family member:
- How do you think you become HIV positive?
- Sexual transmission
- Blood transmission
- Mother to baby transmission
- Did you know about HIV/AIDS before becoming HIV positive?
- Yes
- No
If yes, then please answer your knowledge of the following
- How it spreads – yes/no
- How it does not spread – yes/no
- How it can be prevented – yes/no
- Know places to seek help related to HIV/AIDS – yes/no
- Do you know about HIV/AIDS now?
- Yes
- No
If yes, then please answer your knowledge of the following
- How it spreads – yes/no
- How it does not spread – yes/no
- How it can be prevented – yes/no
- Know places to seek help related to HIV/AIDS – yes/no
- Do you know about Voluntary Counselling and testing?
- Yes
- No
13.Do you know about Antiretroviral Therapy (ART)?
- Yes
- No
14.Do you have access to treatment?
- Yes
- No
15.Do you live with your family?
- Yes
- No
16.If no to question 15, then did your family leave you because of your HIV status?
- Yes
- No
17.Is any member of your family HIV positive or have AIDS?
18.Did you face stigma and discrimination because you have AIDS?
- Yes
- No
19.Did you face verbal abuse?
- Yes
- No
If yes, by whom
20.Did you face physical abuse?
- Yes
- No
If yes, by whom
- Do you think you are fairly treated by Health Care provider?
- Yes
- No
22.Do you think people living with HIV should disclose their HIV status?
- Yes
- No
23.Do you think HIV transmission should be a criminal offence?
- Yes
- No
24.What has been the impact of the criminalisation of HIV transmission on you personally?
25.Do you think criminalisation of HIV transmission affects men and women differently?
26.What is the impact of criminalisation on public health and human rights in your context?
27.Do you think people living with HIV should disclose their HIV status before every sexual encounter? Why/ why not?
APPENDIX – C
UPDATED CV OF THE STUDENT
Particulars of the student:
Name : J. M. Khasru Al Mamun Reza
Father’s name : Md. Shahi Reza
Mother’s name : Khodeza Begum
Permanent address : Village- Kashimpur, Post Office- Jalalpur,
Upazila-Jhenaidah, District- Jhenaidah, Bangladesh.
Present/ Mailing address : Dental Surgeon
Upazila Health Complex, Shailkupa, Jhenaidah.
Date of Birth : 03 January 1977
Marital status : Married
E-mail : reza_mamun09@yahoo.com
: reza.mamun09@gmail.com
Cell phone : +88 01711 041 714
Academic Qualification:
| Exam Title | Institute | Result | Passing Year |
| SSC | Jalalpur high School, Kotchandpur, Jhenaidah. | First Division | 1991 |
| HSC | Govt. M. M College, Jessore. | First Division | 1993 |
| BDS | Chittagong Medical College, Chittagong. | Pass | 2002 |
Job Status:
B.C.S Health Cadre Officer
BCS Batch No. : 24th
Designation : Dental Surgeon
Award/ Achievement:
Director General Award from BIAM Foundation, Dhaka (www.biamfoundation.com) for the 1st position of 26th Special Foundation Training Course for the B.C.S Health Cadre Officers from 25 September to 23 November 2011.