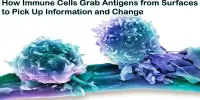
One in every seven men of reproductive age in the world suffers from infertility. Spermatogonial stem cell (SSC) therapy is one treatment option for male sterility. Sperm stem cells from the testis are transferred to a test tube, cultured, and nudged into becoming fully-fledged sperm in this method. However, identifying just the right conditions to get human SSCs to grow in the lab has been a major bottleneck. Many attempts have been made, but in the majority of reported cases, it was unclear whether the cells being cultured was SSCs, and no previously published method is routinely used.
A new study shows that using primate embryonic stem cells, functional sperm cells can be created in a dish. With global rates of male infertility continuing to rise, a new study in spermatogonial stem cell research led by University of Georgia researchers offers hope for future clinical therapies. The research, which was recently published in Fertility and Sterility Science, is the first to demonstrate that functional sperm cells can be created in a dish using primate embryonic stem cells.
“This is a significant step toward developing stem cell-based therapies to treat male infertility in cases where men do not produce any viable sperm cells,” said lead researcher Charles Easley, an associate professor in the University of Georgia’s College of Public Health. Researchers used rhesus macaque embryonic stem cells to generate immature sperm cells known as round spermatids, which they demonstrated could fertilize a rhesus macaque egg.
This is a significant step toward developing stem cell-based therapies to treat male infertility in cases where men do not produce any viable sperm cells.
Charles Easley.
The testes are constantly producing sperm cells, but not all areas of the seminiferous tubules produce sperm cells at the same time. One immature germ cell can take up to 74 days to mature, and there are intermittent resting phases during this process.
The immature cells (called spermatogonia) are all derived from stem cells in the seminiferous tubules’ outer wall. The stem cells are almost entirely made up of nuclear material. (The nucleus is the portion of the cell that contains the chromosomes.) The stem cells begin their process by multiplying through the cell duplication process known as mitosis. Half of the new cells from this initial crop become future sperm cells, while the other half remain as stem cells, ensuring a steady supply of new germ cells. Primary sperm cells are spermatogonia that will develop into mature sperm cells.
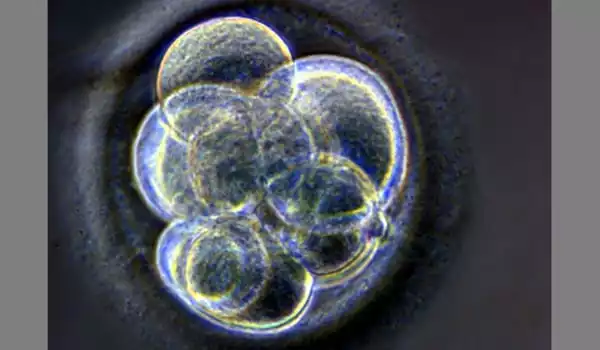
Scientists have been able to generate sperm-like cells from mouse stem cells, according to Easley, but rodent sperm production differs significantly from human sperm production. Until this study, it was unclear whether this technology could ever be used in humans.
“This is the first step in demonstrating that this technology has the potential to be translated. We’re using a more relevant species, and we’re having success creating healthy embryos “Easley stated. Rhesus macaques have reproductive mechanisms that are similar to humans, making them an “ideal and necessary model for exploring stem cell-based therapies for male infertility,” according to the authors.
The cells were differentiated into immature sperm cells known as round spermatids using a novel method developed by the researchers. Fertilization within vitrospermatids, like fertilization with immature spermatids in vivo, requires activating the egg and the addition of other factors to allow the fertilized egg to develop into a healthy embryo.
The researchers intend to implant these embryos into a surrogate rhesus macaque this fall to determine whether these embryos from in vitro spermatids can produce a healthy baby.
If that step is successful, the researchers will repeat the procedure with spermatid-like cells derived from macaque skin cells. Depending on the tissue, adult stem cells can be isolated from the body in a variety of ways. Blood stem cells, for example, can be extracted from a donor’s bone marrow, blood in a baby’s umbilical cord, or circulating blood.
Because these monkeys’ reproductive mechanisms are similar to humans, the researchers used embryonic stem cells from rhesus macaque monkeys to generate immature sperm cells known as round spermatids. These sperm cells were discovered to be capable of fertilizing an egg of a rhesus macaque. Although previous research has demonstrated the ability of mouse stem cells to produce sperm-like cells, this study provides a much clearer picture of the technology’s working potential in humans.