A Novel Therapy against Malaria

Youyou Tu from China Academy of Traditional Chinese Medicine used a compound from a traditional herbal medicine to tackle the challenge of developing novel malaria therapies. She used the plant Artemisia annua and extracted its active component. Tu was the first to show that this component, later called Artemisinin, was highly effective against the malaria parasite, both in infected animals and in humans. Artemisinin represents a new class of antimalarial agents that rapidly kill the malaria parasites at an early stage of their development, which explains its unprecedented potency in the treatment of severe malaria. From a large-scale screen of herbal remedies in Malaria-infected animals, an extract from the plant Artemisia annua emerged as an interesting candidate. Tu was the first to show that this component, later called Artemisinin, was highly effective against the Malaria parasite, both in infected animals and in humans.
Still today, malaria is a widespread disease with more than 3.4 billions people are at risk of contracting Malaria. Malaria infects 200 million individuals annually and in 2012 an estimated 627,000 people died of malaria, most of which were young children in Sub-Saharan Africa. Moreover, in many parts of the world, the parasites have developed resistance to a number of malaria drugs. However, when used in combination therapy, Artemisinin is estimated to reduce mortality from Malaria by more than 20% overall and by more than 30% in children. For Africa alone, this means that more than 100,000 lives are saved each year.
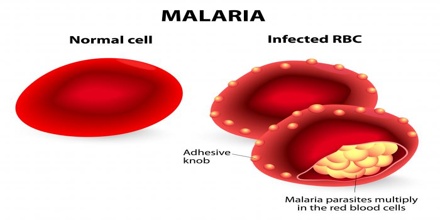
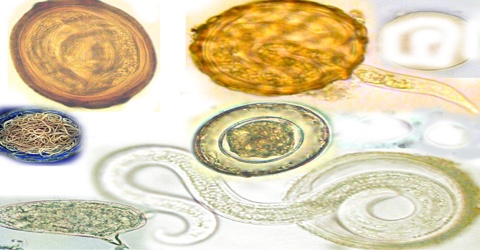
Definition of Malaria
An infectious disease caused by protozoan parasites from the Plasmodium family that can be transmitted by the bite of the Anopheles mosquito or by a contaminated needle or transfusion. Falciparum malaria is the most deadly type.
Malaria transmission occurs primarily between dusk and dawn because of the nocturnal feeding habits of Anopheles mosquitoes. One should therefore take protective measures to reduce contact with mosquitoes, especially during these hours. These measures include remaining in well-screened areas, using mosquito nets, and wearing clothes that cover most of the body.
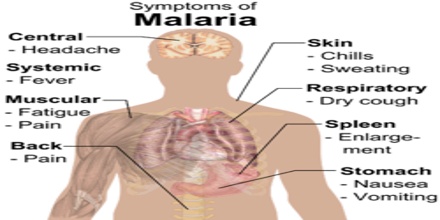
The symptoms of malaria include cycles of chills, fever, sweats, muscle aches and headache that recur every few days. There can also be vomiting, diarrhea, coughing, and yellowing (jaundice) of the skin and eyes. Persons with severe falciparum malaria can develop bleeding problems, shock, kidney and liver failure, central nervous system problems, coma, and die. Travelers to areas with malaria are advised to take medications to prevent infection if exposed. The treatment of malaria is with oral or intravenous medications, including chloroquine, mefloquine (Larium), or atovaquone/proguanil (Malarone).
Treatment and Medication for Malaria
There are several medications available to treat malaria, including
- chloroquine (Aralen);
- Artemether-lumefantrine (Coartem);
- Artesunate-amodiaquine (Amonate);
- Dihydroartemisinin-piperaquine;
- Artesunate-sulfadoxine-pyrimethamine (SP), in areas with known SP sensitivity;
- atovaquone-proguanil (Malarone);
- mefloquine (Lariam);
- quinidine (Quinaglute Dura-Tabs, Quinidex Extentabs, Quin-Release);
- doxycycline (Adoxa, Avidoxy, Acticlate, Doryx, Monodox, Oraxyl, Vibramycin, Vibramycin Calcium, Vibramycin Monohydrate, Vibra-Tabs, used in combination with quinine);
- clindamycin (Cleocin HCl, Cleocin Pediatric, used in combination with quinine);
- artesunate (available only through the CDC).
The choice of drug depends on the species of Plasmodium and if the parasite is drug-resistant. The risk of drug resistance depends on the area where the malaria was acquired. In sub-Saharan Africa, for example, older drugs like chloroquine are largely ineffective.
Most medications are available only as tablets or pills. Intravenous treatment with quinidine may be needed in severe malaria or when the patient cannot take oral medications.