Crohn’s Disease (Symptoms, Diagnosis, and Treatment)
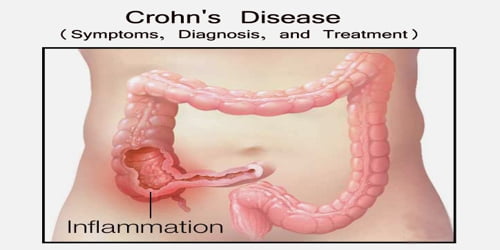
Definition: Crohn’s disease is an inflammatory bowel disease (IBD) that may affect any part of the gastrointestinal tract from mouth to anus. It most commonly occurs in the small intestine and the colon. However, the disease can affect any part of our gastrointestinal (GI) tract, from our mouth to our anus. The disease can involve some parts of the GI tract and skip other parts.
The inflammation caused by Crohn’s disease often spreads deep into the layers of affected bowel tissue. Crohn’s disease can be both painful and debilitating and sometimes may lead to life-threatening complications.
It isn’t clear what causes Crohn’s disease. However, the following factors may influence whether people get it:
- Immune system
- Genetics
- Environment
Up to 20 percent of people with Crohn’s disease also have a parent, child, or sibling with the disease.
Signs and symptoms often include abdominal pain, diarrhea (which may be bloody if inflammation is severe), fever, and weight loss. Other complications may occur outside the gastrointestinal tract and include anemia, skin rashes, arthritis, inflammation of the eye, and tiredness. The skin rashes may be due to infections as well as pyoderma gangrenosum or erythema nodosum.
While there’s no known cure for Crohn’s disease, therapies can greatly reduce its signs and symptoms and even bring about long-term remission. With treatment, many people with Crohn’s disease are able to function well.
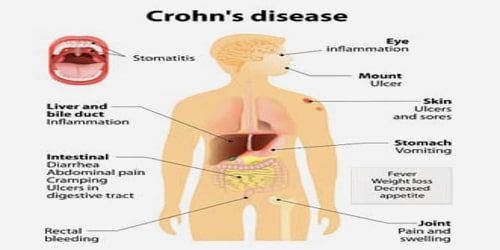
Signs and Symptoms of Crohn’s disease: Signs and symptoms of Crohn’s disease can range from mild to severe. They usually develop gradually, but sometimes will come on suddenly, without warning. They may vary over time and from person to person, depending on what part of the gastrointestinal (GI) tract is inflamed. And because symptoms vary from person to person, the way to gauge what people consider a flare-up of symptoms is relative to what is “normal” for them.
When the disease is active, signs and symptoms may include:
- Diarrhea
- Fever
- Fatigue
- Abdominal pain and cramping
- Blood in people’s stool
- Mouth sores
- Reduced appetite and weight loss
- Pain or drainage near or around the anus due to inflammation from a tunnel into the skin (fistula)
Other signs and symptoms –
People with severe Crohn’s disease also may experience:
- Inflammation of skin, eyes, and joints
- Inflammation of the liver or bile ducts
- Delayed growth or sexual development, in children
Crohn’s can affect the entire GI tract — from the mouth to the anus — and can be progressive, so over time, people’s symptoms could get worse. That’s why it’s important that they have an open and honest conversation about their symptoms since the doctor will use that information to help determine what treatment plan is best for them.
Diagnosis and Treatment of Crohn’s disease: The diagnosis of Crohn’s disease can sometimes be challenging, and a number of tests are often required to assist the physician in making the diagnosis.
There is no one test to diagnose Crohn’s disease. The doctor will likely use a combination of tests to help confirm a diagnosis of Crohn’s disease, including:
Blood tests may include:
- Antibody tests
- Complete blood count (CBC)
- C-reactive protein
- Electrolyte panel
- Erythrocyte sedimentation rate
- Iron and B12 levels
- Liver function
Procedures:
- Colonoscopy
- Computerized tomography (CT)
- Magnetic resonance imaging (MRI)
- Capsule Endoscopy
- Balloon-assisted enteroscopy
Other conditions with similar symptoms as Crohn’s disease include intestinal tuberculosis, Behçet’s disease, ulcerative colitis, nonsteroidal anti-inflammatory drug enteropathy, irritable bowel syndrome, and celiac disease.
Even though there is currently no cure for Crohn’s disease, there is a wide range of treatment options available that can help control Crohn’s symptoms and even help people achieve and maintain remission (having few or no symptoms over a period of time) as long as they stay on their treatment as prescribed. In fact, achieving and maintaining remission is the main goal of Crohn’s disease treatment.
- Medication for Crohn’s disease: Several types of medications are available to treat Crohn’s disease. Medications used to treat the symptoms of Crohn’s disease include 5-aminosalicylic acid (5-ASA) formulations, prednisone, immunomodulators such as azathioprine (given as the prodrug for 6-mercaptopurine), methotrexate, infliximab, adalimumab, certolizumab, vedolizumab, and natalizumab. Hydrocortisone should be used in severe attacks of Crohn’s disease.
- Surgery: However, surgery may be a consideration if the disease doesn’t respond to medication—although surgery is not a cure for Crohn’s disease, as it is sometimes considered to be in ulcerative colitis. In fact, about 60%-75% of Crohn’s patients may require surgery at some point to correct potential complications of Crohn’s disease—such as clearing an intestinal blockage or repairing damage to the intestines. Damage to the intestines can include a perforation or abscess (a pus-filled area caused by infection).
- Lifestyle changes: Certain lifestyle changes can reduce symptoms, including dietary adjustments, elemental diet, proper hydration, and smoking cessation. Diets that include higher levels of fiber and fruit are associated with reduced risk, while diets rich in total fats, polyunsaturated fatty acids, meat, and omega-6 fatty acids may increase the risk of Crohn’s. Smoking may increase Crohn’s disease; stopping is recommended. Eating small meals frequently instead of big meals may also help with a low appetite.
The benefits of surgery for Crohn’s disease are usually temporary. The disease often recurs, frequently near the reconnected tissue. The best approach is to follow surgery with medication to minimize the risk of recurrence.
Information Source: