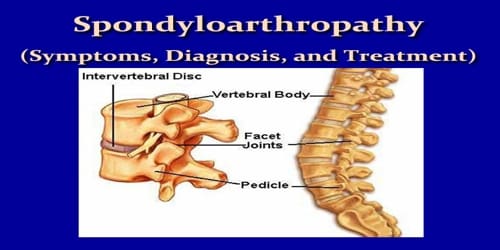
Spondyloarthropathy (Symptoms, Diagnosis, and Treatment)
Definition: Spondyloarthropathy or spondyloarthrosis refers to a group of inflammatory rheumatic diseases that includes ankylosing spondylitis and psoriatic arthritis. They can cause pain and sometimes damage joints like our backbone, shoulders, and hips.
As such, it is a class or category of diseases rather than a single, specific entity. It differs from spondylopathy, which is a disease of the vertebra itself. However, many conditions involve both spondylopathy and spondyloarthropathy.
The predominant symptom among them is joint pain and inflammation, sometimes affecting the spine. In some cases, these diseases can become systemic, causing inflammation in the eyes, gastrointestinal tract, and skin.
Like many other chronic conditions, spondyloarthritis symptoms may come and go. Symptoms may also vary from day to day. Complications, such as heart problems and lung scarring due to long-term inflammation, are rare.
These diseases have the following conditions in common:
- Seronegative (i.e. rheumatoid factor is not present)
- They are in relation to HLA-B27
- Inflammatory axial arthritis, generally sacroiliitis and spondylitis
- Oligoarthritis, generally with an asymmetrical presentation
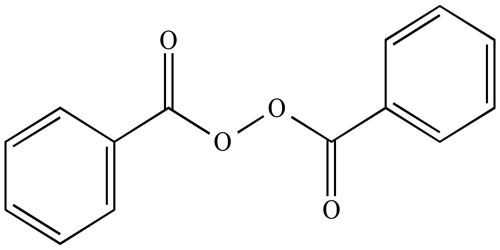
- Enthesitis (inflammation of the entheses, the sites where tendons or ligaments insert into the bone.), e.g. Plantar fasciitis, Achilles tendinitis, costochondritis.
- Familial aggregation occurs
- Extra-articular features, such as involvement of eyes (anterior uveitis), skin, genitourinary tract, and aortic regurgitation
- Overlap is likely between several of the causative conditions
Spondyloarthropathies have been linked to several genes; some experts believe that a combination of genetic and environmental factors may trigger their development.
Worldwide prevalence of spondyloarthropathy is approximately 1.9%.
Signs and Symptoms of Spondyloarthropathy: The main symptoms of spondyloarthritis are the pain, stiffness, and swelling. Bone damage may also occur. Where people feel symptoms in the body depends on the type of spondyloarthritis they have.
Back pain is the most common symptom of a spondyloarthropathy. But there are a variety of other symptoms that might point to an illness of this type:
- Joints like our hips, shoulders, knees, or elbows are painful and swollen.
- The points where our tendons and ligaments meet bone become inflamed. This is called enthesitis. The first sign is usually a pain at the back or bottom of our heels.
- Dactylitis is an inflammation of the tendons in the fingers and toes. This gives them a swollen, sausage-like appearance.
- Uveitis causes pain or redness in one eye.
- Other possible signs are a skin rash associated with psoriasis or an inflammatory intestinal illness.
People with ankylosing spondylitis sometimes develop arthritis in their hips and shoulders early on. It also can make people feel fatigued or lose their appetite. People might run a mild fever.
Diagnosis and Treatment of Spondyloarthropathy: Early diagnosis is important to help manage symptoms and reduce people’s risk of complications or disability. The doctor may suspect people have spondyloarthritis based on their symptoms, medical history, and a medical exam. Testing will be necessary to come to a formal diagnosis and may include:
- X-rays: Changes in the sacroiliac joints—the joints connecting the sacrum and the top of the pelvis—are often a key sign of spondyloarthritis.
- Magnetic resonance imaging (MRI): If X-ray results are not clear; an MRI may show the signs more accurately.
- Blood tests: A blood test can determine whether you have the HLA-B27 gene. (Having the gene, however, does not necessarily mean people will develop spondyloarthritis.)
There are no known cures, but the doctor can help people manage their condition. Treatment will likely involve a rheumatologist. This is a doctor who specializes in treating diseases like arthritis.
Treatment plans are individualized, but most will include:
- physical therapy
- low-impact exercise
- non-steroidal anti-inflammatory drugs
- corticosteroid injections
- antirheumatic drugs
- TNF alpha-blocker drugs
Antibiotics are used to treat an active bacterial infection present with reactive arthritis. Severe cases of spondyloarthritis may require surgery to treat bone destruction or cartilage damage.
In some cases, spinal surgery may be needed to relieve pressure on the vertebrae; this is most common with ankylosing spondylitis. When inflammation destroys the cartilage in the hips, surgery to replace the hip with a prosthesis, called total hip replacement, can relieve pain and restore the joint’s function.
Regular exercise and physical therapy go a long way to support mobility and reduce stiffness and pain. Over-the-counter and prescription medications to reduce inflammation are also often beneficial.
Information Source: