Ulcerative Colitis (Symptoms, Diagnosis, and Treatment)
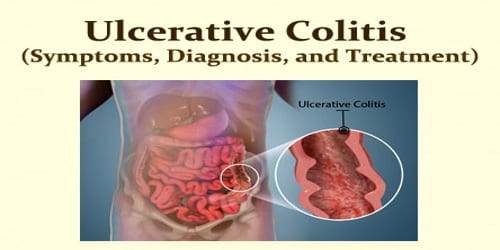
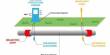
Definition: Ulcerative colitis (UC) is a fairly common chronic, or long-term, disease that causes inflammation of the large intestine (also called the colon). It is a form of inflammatory bowel disease (IBD) that has some similarity to Crohn’s disease. The colon, or large intestine, removes nutrients from undigested food and gets rid of waste products through the rectum and anus when we pass feces.
Ulcerative colitis inflammation may cause abdominal pain, diarrhea and other symptoms that vary from person to person and from mild to severe. Symptoms typically occur intermittently with periods of no symptoms between flares. Complications may include megacolon, inflammation of the eye, joints, or liver, and colon cancer.
While this disease affects people of all ages, most people are diagnosed between the ages of 15 and 35. After age 50, another small increase in diagnosis for this disease is seen, usually in men.
The exact cause of ulcerative colitis remains unknown. Previously, diet and stress were suspected, but now doctors know that these factors may aggravate but don’t cause ulcerative colitis. Researchers believe ulcerative colitis is caused by a combination of factors that involve genetics, the environment, and an overactive immune system.
Several medications are used to treat symptoms and bring about and maintain remission, including aminosalicylates such as mesalazine or sulfasalazine, steroids, immunosuppressants such as azathioprine, and biologic therapy.
Doctors often classify ulcerative colitis according to its location. Types of ulcerative colitis include: Ulcerative proctitis, Proctosigmoiditis, Left-sided colitis, Pancolitis, and Acute severe ulcerative colitis.
The disease is more common in North America and Europe than in other regions. Often it begins in people aged 15 to 30 years, or among those over 60. Males and females appear to be affected in equal proportions. With appropriate treatment, the risk of death appears the same as that of the general population.
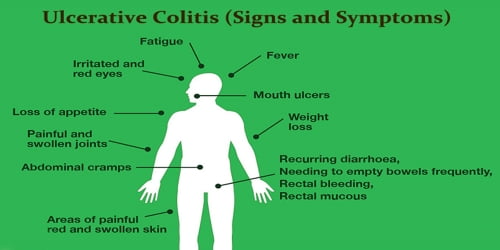
Signs and Symptoms of Ulcerative Colitis: Ulcerative colitis symptoms can vary, depending on the severity of inflammation and where it occurs. Symptoms may vary over time and from person to person, depending on what part of the large intestine is inflamed and the severity of the inflammation.
Common symptoms of ulcerative colitis include:
- abdominal pain
- increased abdominal sounds
- bloody stools
- diarrhea
- fever
- rectal pain
- weight loss
- malnutrition
Ulcerative colitis (UC) may cause additional conditions such as:
- joint pain
- joint swelling
- nausea and decreased appetite
- skin problems
- mouth sores
- eye inflammation
- tenesmus: a sudden and constant feeling that people have to move their bowels
Most people with ulcerative colitis have mild to moderate symptoms. The course of ulcerative colitis may vary, with some people having long periods of remission.
Ulcerative colitis is unpredictable and can be progressive (get worse). Over time, people’s symptoms may change in severity or change altogether. People may go through periods of remission—when they have few or no symptoms. Their symptoms may also come on suddenly, without warning.
Diagnosis and Treatment of Ulcerative Colitis: A doctor will ask about symptoms and medical history, and try to find out whether any close relatives have had ulcerative colitis, IBD, or Crohn’s disease. They will also examine the patient for signs of anemia and tenderness in the abdominal area.
This disorder mimics other bowel diseases such as Crohn’s disease. The doctor will run multiple tests to rule out other conditions. Tests to diagnose ulcerative colitis often include:
- blood tests
- stool tests
- x-ray
- barium enema
- sigmoidoscopy, in which a flexible tube with a camera at the end is inserted through the anus into the rectum
- colonoscopy, where a long, flexible viewing tube with a camera at the end is inserted through the anus and the rectum
- CT scan of the abdomen or pelvis
Although ulcerative colitis is a disease of unknown causation, an inquiry should be made as to unusual factors believed to trigger the disease. The simple clinical colitis activity index was created in 1998 and is used to assess the severity of symptoms.
Fortunately, there is a wide range of treatment options available that can help control ulcerative colitis (UC) as long as people stay on their treatment as prescribed. Getting ulcerative colitis under control and achieving remission (few or no symptoms) is the main goal of ulcerative colitis treatment.
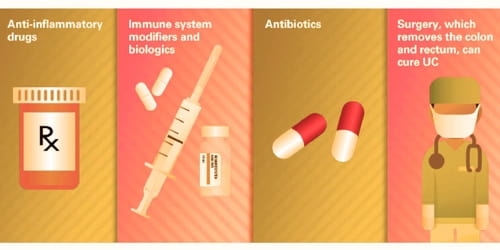
Ulcerative colitis treatment usually involves either drug therapy or surgery.
Medication: Ulcerative colitis can be treated with a number of medications, including 5-ASA drugs such as sulfasalazine and mesalazine. Corticosteroids such as prednisone can also be used due to their immunosuppressive and short-term healing properties, but because their risks outweigh their benefits, they are not used long-term in treatment. Immunosuppressive medications such as azathioprine and biological agents such as infliximab and adalimumab are given only if people cannot achieve remission with 5-ASA and corticosteroids.
Vedolizumab (Entyvio) medication was recently approved for the treatment of ulcerative colitis for people who don’t respond to or can’t tolerate other treatments. It works by blocking inflammatory cells from getting to the site of inflammation.
Surgery: If other treatments do not work, surgery may be an option.
- Colectomy: The colon, or part of it, is removed.
- Ileostomy: The surgeon makes an incision in the stomach, and the end of the small intestine is extracted and connected to an external pouch. The pouch collects waste material from the intestine.
- Ileoanal pouch: The pouch is constructed by the surgeon internally, out of the small intestine, and then connected to the muscles surrounding the anus. The ileoanal pouch is not an external pouch.
A type of leukocyte apheresis, known as granulocyte and monocyte adsorptive apheresis, still requires large-scale trials to determine whether or not it is effective. Results from small trials have been tentatively positive.
Information Source: