Introduction
Blood is a specialized fluid connective tissue in which there are liquid intercellular substances (plasma) and formed elements (RBC, WBC, Platelet) suspended in the plasma which circulates in closed system of blood vessels. it is red thick and slightly alkaline1
The normal total circulating blood volume is about 8% of the body weight (5600 ml in a 70 kg man). About 55% of this volume is plasma and 45% is cellular element that is composed of WBC, RBC, and Platelet that suspended in the plasma. 2
Structurally the simplest cell in the body, volumes have been written about the lower red blood cell. The basic function of the RBC is the creation and maintenance of an environment salutary to the physical integrity and functionality of hemoglobin. In the normal state, erythrocytes are produced only in the skeleton (in adults only in the axial skeleton), but in pathologic states (especially myelofibrosis, which will be covered subsequently) almost any organ can become the site of erythropoiesis. Numerous substances are necessary for creation of erythrocytes, including metals (iron, cobalt, manganese), vitamins (B12, B6, C, E, foliate, riboflavin, pantothenic acid, thiamin), and amino acids. Regulatory substances necessary for normal erythropoiesis include erythropoietin, thyroid hormones, and androgens. Erythrocytes progress from blast precursors in the marrow over a period of five days. Then they are released into the blood as reticulocytes, distinguishable from regular erythrocytes only with special supravital stains. The reticulocyte changes to an erythrocyte in one day and circulates for 120 days before being destroyed in the reticuloendothelial system.
Also referred to as just “RBC,” this simply involves counting the number of RBC per unit volume of whole blood. Manual methods using the hated hemocytometer have been universally replaced by automated counting. The major source of error in the RBC count is an artificially reduced result that occurs in some conditions where RBC stick together in the sample tube, with two or more cells being counted as one. The result of the test is expressed as number of cells per unit volume, specifically cells/µL. A typical lab’s normal range is 4.2 – 5.4 x 106/µL for females; for adult males it is 4.7 – 6.1 x 106 /µL.3 Hemoglobin, also spelled haemoglobin and abbreviated Hb, is the iron-containing oxygen-transport metalloprotein in the red blood cells of the blood in vertebrates and other animals. In mammals the protein makes up about 97% of the red cell’s dry content, and around 35% of the total content (including water). Hemoglobin transports oxygen from the lungs or gills to the rest of the body, such as to the muscles, where it releases its load of oxygen. Hemoglobin also has a variety of other gas-transport and effect-modulation duties, which vary from species to species, and may be quite diverse in invertebrates.
The name hemoglobin is the concatenation of heme and globin, reflecting the fact that each subunit of hemoglobin is a globular protein with an embedded heme (or haem) group; each heme group contains an iron atom, and this is responsible for the binding of oxygen. The most common type of hemoglobin in mammals contains four such subunits, each with one heme group. In humans, each heme group is able to bind one oxygen molecule, and thus, one hemoglobin molecule can bind four oxygen molecules.4
The normal range for hemoglobin is highly age- and sex-dependent, with men having higher values than women, and adults having higher values than children (except neonates, which have the highest values of all). For a typical clinical lab, the young adult female normal range is 12 – 16 g/dl; for adult males it is 14 – 18 g/dl.5
Hemoglobin (Hb) is synthesized in a complex series of steps. The heme portion is synthesized in a series of steps which occur in the mitochondria and the cytosol of the immature red blood cell, while the globin protein portions of the molecule are synthesized by ribosomes in the cytosol [3]. Production of Hb continues in the cell throughout its early development from the proerythroblast to the reticulocyte in the bone marrow. At this point, the nucleus is lost in mammalian red blood cells, but not in birds and many other species. Even after the loss of the nucleus in mammals, residual ribosomal RNA allows further synthesis of Hb until the reticulocyte loses its RNA soon after entering the vasculature (this hemoglobin-synthetic RNA in fact gives the reticulocyte its reticulated appearance and name).
Decrease of hemoglobin, with or without an absolute decrease of red blood cells, leads to symptoms of anemia. Anemia has many different causes, although iron deficiency and its resultant iron deficiency anemia are the most common causes in the Western world. As absence of iron decreases heme synthesis, red blood cells in iron deficiency anemia are hypochromic (lacking the red hemoglobin pigment) and microcytic (smaller than normal). Other anemias are rarer. In hemolysis (accelerated breakdown of red blood cells), associated jaundice is caused by the hemoglobin metabolite bilirubin, and the circulating hemoglobin can cause renal failure9 Anemia is present when the hemoglobin level in the blood is below the lower extreme of normal range for the age and sex of the individual. The lower limit of normality is reduced during pregnancy. 10
Anemia can be caused by many things, but the three main bodily mechanism that produces it are: excessive destruction of RBC, blood loss, inadequate production of RBCs.11
Clinical manifestations of anemia are symptoms like fatigue, tierdness, effort intolerance, effort dyspnoea, and palpitaions
Signs are pallor, high cardiac output state, and congestive cardiac failure. 10
Anemia is usually classified according to etiology, path physiology & morphology
MORPHOLOGIC CLASSIFICATION of Anaemia
- Macrocytic
- MCV > 100 MCH and MCHC normal
- Normocytic
- MCV > normal MCH and MCHC normal
- Simple microcytic
- MCV < 80 MCH and MCHC normal
- Microcytic hypochromic
- MCV < 80 MCH and MCHC decreased
Microcytic Anemia
These are associated with an inability to produce hemoglobin. Hemoglobin
consists of iron inserted into the prtoporphyrin ring complex to form heme
which in turn is inserted into the globin chain? Hence these anemia’s
are seen in:
Iron deficiency – absence of iron, chronic disease – iron unavailable, thalassemia – inability to produce globin chains & sideroblastic anemia- inability to produce heme12
Iron deficiency anemia is the most common type of anemia, and the most common cause of anemia. Iron deficiency anemia occurs when the dietary intake or absorption of iron is
insufficient, and hemoglobin, which contains iron, cannot be formed. The principal cause of iron deficiency anemia in premenopausal women is blood lost during menses.13
The hereditary disorder of hemoglobin may be classified two broad groups, the hemoglobinopathies and the thalassaemias.The hemoglobinopathies are characterized by the production of structurally defective hemoglobin due to abnormallities in the formation of the globin moiety of the moelcule.the thallasaemia are characterized by a reduced rate of production of normal hemoglobin due to absent or decreased synthesis of 1 or more types of globin polypeptide chains. The thalassaemias are wide spread with maximam prevalence arround the Mediterranean littoral and in south East Asia11
Risk factors are conditions or behaviors that increase chances of developing diseases, Iron deficiency is more frequent in women who smoke, eat a diet low in iron and have heavy periods In adults the most common cause is losing blood faster than the body can replace it. A lack of iron in the diet is common in vegans and vegetarians because the main dietary source is red meat, babies can develop iron deficiency, especially if they are premature. Storing iron is not usually completed until the final stages of pregnancy, the body needs more iron when a large amount of cell divisions occur, such as in pregnancy and during periods of rapid childhood growth, loss of blood through heavy menstruation can deplete iron stores, diseases of the small intestine such as gluten intolerance (coeliac disease) and Crohn’s disease (inflammation of the intestine) can reduce its ability to absorb iron, gender discrimination, illiteracy, poor economic status.12
A combination of these factors possibly contributes to the low level of awareness, treatment and control of anaemia in our country. This is a community study with descriptive nature. This was cross-sectional in pattern of time and approach to the study subjects. For this study standards were set according to the World Health Organization set criteria for research.13
Following measures should be taken to maintain the normal level of Hb in young adults: Eat a varied, well-balanced diet that contains foods from all the food groups (protein,
carbohydrate, fat, fruit, and vegetables). Good sources of iron include liver, beef, whole meal bread, cereals, eggs and dried fruit. If you often get heavy periods, it’s a good idea to seek medical advice because you may be at risk of anaemia. If you are pregnant or planning to become pregnant, talk to your doctor about iron supplements. Hence public education to overcome such problem and promote healthy behaviors is essential and should be directed towards the individual and the community, and should start early in childhood.14
Bangladesh, on the northern coast of the Bay of Bengal, is surrounded by
India, with a small common border with Myanmar in the southeast. Bangladesh is a developing country of the world. Area is about 56,977 square miles and population 124 million. According to statistical year book 2001, gross national income per capita is US $ 375.Along with high birth rate and lower literacy level most of the people lies below the poverty line. So many of our young adult suffering from nutritional deficiency. Such as anemia, PEM etc. On the background of Bangladesh, the cause of nutritional deficiency mainly are poverty, lack of proper knowledge, high birth rate, unhealthy mother
give birth unhealthy baby.15
The normal Hb level of young adult range is Female 12-16 gm/dl & Male 14-18 gm/dl. Most of our young adults in Bangladesh are anaemic due to their Hb level in
the blood is below normal range. Anemia one of the more common blood
disorder, occurs when the level of healthy red blood cell in the body becomes too low. This can lead to Health problem because RBCs contain Hb, which carries Oxygen to the body’s tissues. The body needs iron, vitamin B12 and folic acid to produce more red blood cells. If there is a lack of one or more of these nutrients, anemia will develop. Iron deficiency anemia is the most common type of anemia. Anemia can cause a variety of complications, Including fatigue and stress on bodily organs. A lack of iron in the diet is common in vegans and vegetarians because the main dietary source is red meat. Babies can develop iron deficiency, especially if they are premature. Storing iron is not usually completed until the final stages of pregnancy. The body needs more iron when a large
amount of cell divisions occur, such as in pregnancy and during periods of rapid childhood growth. Loss of blood through heavy menstruation can deplete iron stores. The young generation is the future of our country.
They are the prime mover of development. So they should have awakened about their health & nutrition and also take precaution such as: Iron tablet will rapidly reverse anemia, so long as any underlying cause of blood loss has been treated. The tablets can irritate the stomach and should be taken after food to prevent this. There may be a need for intramuscular iron injections to be given instead of tablets, but this is far less common. So many of them are severely malnourished and unhealthy. These conditions increase their malleability to disease and reduce child’s chance of proper nutrition and health. Good nutrition is the cornerstone for survival, health and development for current and succeeding generations. Well-nourished children perform better in school, grow into healthy adults and in turn give their children a better start in life. Well-nourished women face fewer risks during pregnancy and childbirth, and their children set off on firmer under nutrition is implicated in more than half of all child death worldwide. Under nourished children have lowered resistance to infection; they are more likely to die from common childhood ailments like diarrhoeal diseases and respiratory infections, and for those who survive, frequent illness saps their nutritional status, locking them into a vicious cycle of recurring sickness and faltering growth. Their plight is largely invisible: three quarters of the children who die from causes related to malnutrition were only mildly or moderately undernourished, showing no outward sign of their vulnerability.evelopmental paths, both physically and mentally. Malnutrition is a complex condition that can involve multiple, overlapping deficiencies of protein, energy and micronutrients — so called because they are nutrients needed by the body in only tiny amounts. A child becomes malnourished because of illness in combination with inadequate food intake. Insufficient access to food, poor health services, the lack of safe water and sanitation, and inadequate child and maternal care. Inadequate care for children and women is an underlying cause of malnutrition only recently recognized in all its harmful ramifications. Good hygiene in and around the home and in handling food reduces the risk of illness. Care also includes all interaction between parent and child that helps children develop emotionally as well as physically. Several studies have found that malnourished children who were stimulated verbally and cognitively had higher growth rates than those who were not. UNICEF supplied a total of 2.7 billion iron/foliate tablets to 122 countries between 1993 and 1996 for distribution among pregnant women to help reduce iron deficiency anaemia and foliate deficiency. Wheat flour is being fortified with iron in a number of countries in Latin America and the Middle East. Nutrition promoters in Bangladesh are working in 1,000 community centers to help support breastfeeding and better caring practices for women and children. Breastfeeding is the foundation of good nutrition for infants, and inadequate breastfeeding can jeopardize infants’ health and for their normal growth and development of body. In Bangladesh, most of the people suffer from microcytic hypocromic anemia. This may be due to the presence of sub clinical iron deficiency. Both clinical and sub clinical iron deficiency constitute one of the most frequently encountered nutritional anemia and the prevalence of iron responsive microcytic hypocromic anemia varies from 9-70% in different population group. The incidence being higher in the less developed countries compared to the nation of the world. In the United States and Canada the prevalence of microcytic hypocromic anemia
Was reported to the range from 2.3%-27%.There are several causes of iron deficiency including many parasitic disease and other infection, consumption of highly refined food, Use of aluminum and steel cookware rather than iron utensils, lower intake of iron rich food, particularly vegetables and gastrointestinal disorder loading to impaired iron absorption. Hemoglobin level of the people depends on their socio economic condition, literacy level and awareness. There is a direct proportional relationship between higher education level of people and hemoglobin level of them. So it can be suggested that hemoglobin level can be improved by increasing literacy rate and awareness of the people, consciousness about their personal hygiene, and food habit may play an important role in this regard.
Discussion
The study of haematological parameter of university level students was carried out 4th April to 20th June, 2007.
The present study was conducted among students of DhakaNationalMedicalCollege. They were interviewed and examined as per interview schedule. Necessary information as history, general examination and clinical findings were collected from questionnaire and blood examination reports of the pathology department. The following important findings are found from this study.
We investigated the young students of DhakaNationalMedicalCollege of middle and effluent socioeconomic background of Dhaka, capital of Bangladesh. The population are generally healthy .The study has covered the students of age 1st, 2nd and 3rd year MBBS students ranging from (19-22) years separately in the males and females, to determine the value of haematological parameter The study reveals that majority of the respondents passes normal haematological parameter and occurrence of other diseases is also low. This is as the respondents come from affluent family background.
In this study majority of the respondents (70.77%) belongs to 19-20 age group and 29.23% are belongs to 21-22 age group, 69.23% are male and 30.77% are female,87.69% are Muslims and 12.31% are Hindus .63.08% of the respondents have normal range of BMI and 26.15% indicate as grade-1 obesity.75% of the female respondents have normal menstrual history and 25% have dysmenorrhea, regarding general examination of the respondents 96.93% are normal and 3.07% have pallor.
The mean haemoglobin level of majority of female in our study was 12-16gm/dl (mean 14gm/dl) and for male 12-16gm/dl (mean 14 gm/dl).In this study by GuytonAB ct.at it was 14.0 gm/dl for male and 12.45 gm/dl for females of urban black African, which is similar to our study.23
The mean total count of WBC of our study is 4-11X 109 /L. In study by Mohsen A.F. EL Hazmi it was 5-9×109/L among the adolescents of Saudi. The WBC count is near about similar in comparison to some country as in Nigeria, where WBC count was 5-12X109/L.13
The BMI of majority of respondents in our study belongs to (18.5-24.99). On the other hand again in the study by Professor Dr. El Hazmi it was (17.0-29.99) in the young adults of Saudi adolescents and children. The BMI is also similar in comparison to India, Pakistan, where BMI was (17.6-26.65).30
Hemoglobin levels of 34% have 14-14.9gm/dl, 25% belongs to 15-15.9m/dl, and 17% belongs to 12-12.9 gm/dl. 6 of the female respondents have lower hemoglobin level than that of normal (<12gm/dl). 90.769% of the respondents pass normal. ESR (5-20 mm in 1st hour) and 9.231% belongs to >20mm in 1st hour. Extensive studies during the last 3-4 decades conducted in different population have worked out normal reference ranges for hematological parameters in adults and children and have reported significant differences in different ethnic gr.In African-American, African and Afro-Caribbean children ,the levels of these parameters are generally lowers than in Caucasians environmental factors and altitude also influence the value of hematological parameters33.
In the present study, we found that, the male values are higher than the female values. We found 6 female (9.23%) whose hemoglobin level are below normal <12gm/dl. This may be due to menstrual loss of iron, loss dietary intake and increased iron requirement in this age (19-22 year).
In Bangladesh most of the people suffers from microcytic hypo chromic anemia. One of the most frequently encountered nutritional anemias and the prevalence of iron responsive microcytic hypo chromic anemia varies from 9-70 % in different population group.The compared to the developed nation of the world. In the United States and Canada the prevalence of microcytic hypo chromic anemia was reported to the range from 2.3%-27%.
Operational definition:
Blood: Blood is a specialized fluid connective tissue in which there is liquid intercellular substance (Plasma) & formed elements (RBC, WBC & Platelets) suspended in the plasma which circulates in closed system of blood vessels. It is red, thick & slightly alkaline.
Volume – 4 to 5 liter
Hemoglobin: Hemoglobin is the main consultant of red cell & is a red globular protein molecule. Normal range of hemoglobin-
Male : 13-18 gm/dl.
Female: 11.5- 16.5 gm/dl.
Full term body (cord blood): 13.5-19.5 gm/dl
Children (1 year): 11-13 gm/dl
Children (10-12 yr):11.5-14.5 gm/dl.
Anemia: A reduction in the number of circulating RBC per cubic millimeter, the amount of Hemoglobin per 100 ml of blood, below the normal range appropriate for age & sex. In adult male when Hemoglobin is less than 13 gm/dl & in female less than 11.5 gm/dl it is labeled as anemia.
Mild anemia : Hemoglobin up to 11 gm/dl
Moderate anemia : Hemoglobin – 9 to11gm/dl
Severe : Hemoglobin – below 9 gm/dl
ESR: (Erythrocyte Sedimentation Rate)
When a sample of venous blood is mixed with a suitable anticoagulant (citrated blood) and kept standing in a narrow vertical tube the red cell settle down gradually to the bottom of the tube leaving clear plasma above. The rate in millimeters at which the red blood cells are settled down at the end of first hour is called ESR.
WBC: White blood cells are the color less nucleated cell of the blood which is the mobile units of the body’s protective system.
Neutrophils: Multi lobed nucleus (3-5 lobes) connected by chromatin filaments. Cytoplasmic granules are fine, pinkish blue granules distributed uniformly.
Eosinophils: 2-3 lobed nucleus, cytoplasmic granules is coarse brick red to orange , uniformly distributed.
Basophil: Nucleus is multi lobed.Cytoplasmic granules very coarse granules, stain deep purple, not uniform.
Monocyte: Large eccentric nucleus which is kidney shaped. Cytoplasmic granules is absent, pale grey blue cytoplasm.
Lymphocytes: Large round nucleus. Thin crescent of clear blue cytoplasm no granules.
RBC: Red blood cell is a bag of hemoglobin. It has no nucleus but it has hemoglobin. RBC is circular, biconcave, non-nucleated, disk shaped.
Red Cell Indices:
MCV: Mean Corpuscular volume is the average volume or size of the RBC. If the MCV is less than 80 ft then it is microcytic and macrocytic when MCV is more than 95ft.
MCH: Mean corpuscular hemoglobin is the mean amount of hemoglobin per red cell.
MCHC: Mean corpuscular hemoglobin concentration is the mean concentration of the hemoglobin within the red cell.
Microcytic Hypo chromic anemia: MCV, MCHC & MCH are below normal. Eg: iron deficiency anemia of chronic (most common anemia), thalassaemia, anemia of chronic diseases & sideroblastic anemia.
Blood pressure: The tension exerted by blood against arterial walls. De4termining factors include ventricular contraction, arteriolar & capillary resistance, elasticity of the arterial walls, blood volume & viscosity.
Normal level:-
Systolic- 110-140 mm of Hg
Diastolic – 60-90 mm of Hg
Blood mass index (BMI): An index for estimating obesity obtained by dividing wt, in kg by height in meters squared
Weight in Kg
BMI = Height in meter2 X 100
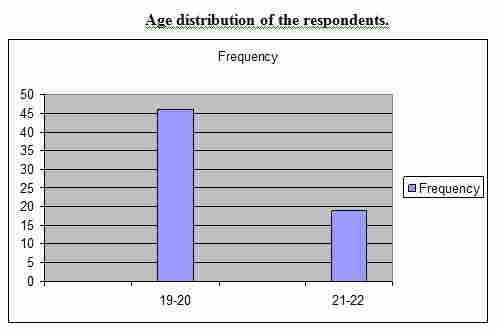
Figure no 1
Age distribution of the respondents.
Above table shows that according to the age of the respondents majority (70.77%) belongs to 19-20 age group, 29.23% belongs to 21-22 age group.
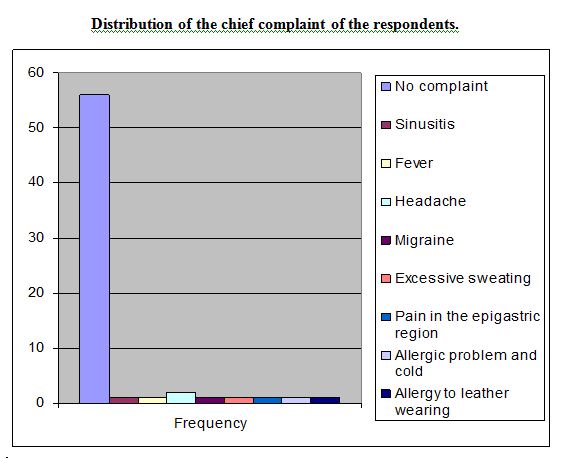
Figure no 2
Distribution of the chief complaint of the respondents.
Above table shows that majority of the respondents (86.15%) have no complain of disease and 3.1% have complain of headache .
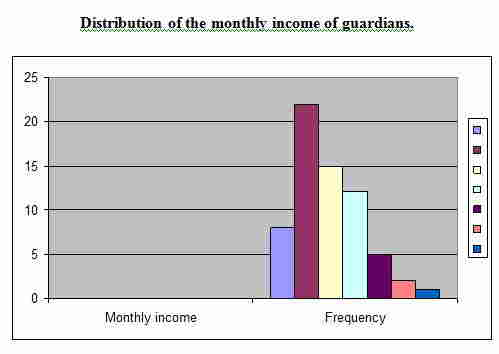
Figure no 3
Distribution of the monthly income of guardians.
Conclusion
The aim of the study is to evaluate the routine blood examination result of adult male and female of under graduate level students. Hemoglobin level of 33.846% belongs to 14-14.9; 24.71% belongs to 15-15.9 and 16.923% belongs to 12-12.9. 9.23% of the respondents, those are female have hemoglobin level <12 gm/dl. ESR of majority 90.769% respondents belongs to 5-20and 9.231% belongs to (>20).
As far as the study reveals, the study shows the hemoglobin level of the respondents depends on their socio economic condition, literacy level and awareness. There is a direct proportional relationship between higher education level of respondents and hemoglobin of them. On the basis of the findings, it can be suggested that hemoglobin level can be improved by increasing literacy rate and awareness of the respondents.
It can be mentioned that this study only indicates the hemoglobin status of the students of Dhaka national medical college; not the whole country.Neverthless, considering the findings of this study it can be conducted that the hemoglobin status of the students of Dhaka national medical college is satisfactory and encouraging.